Spine Dissection
Lab Summary
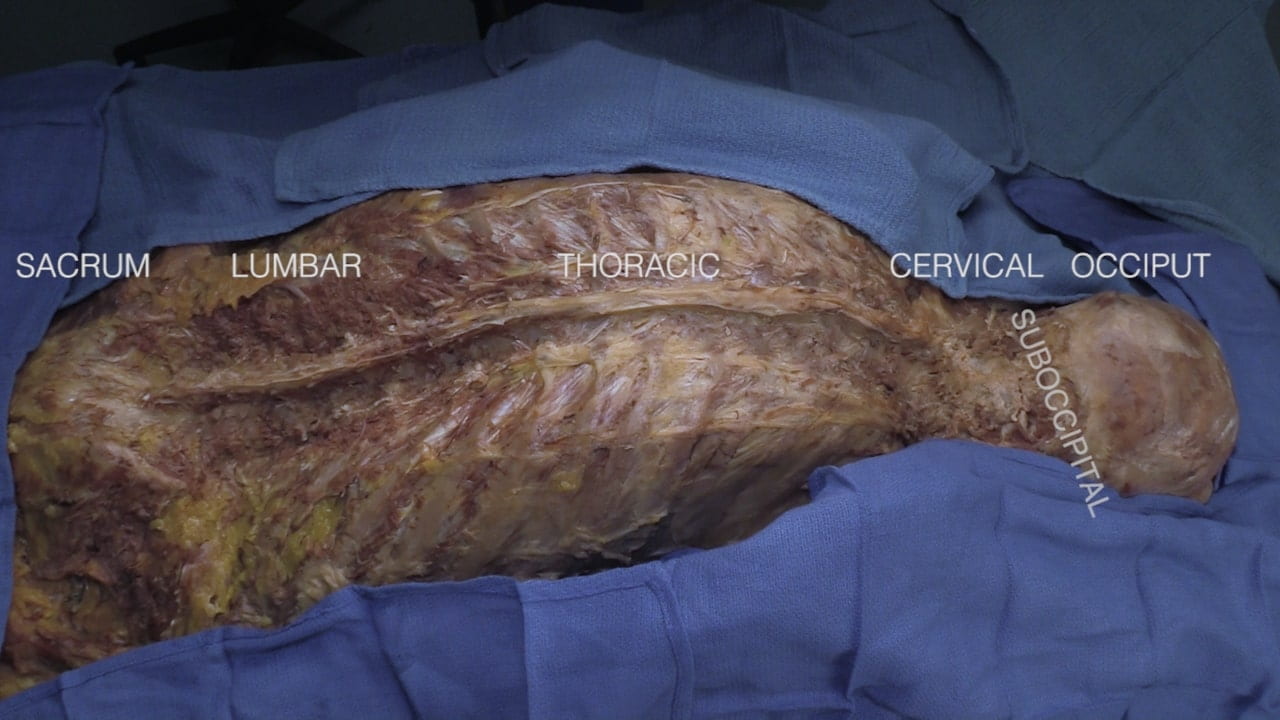
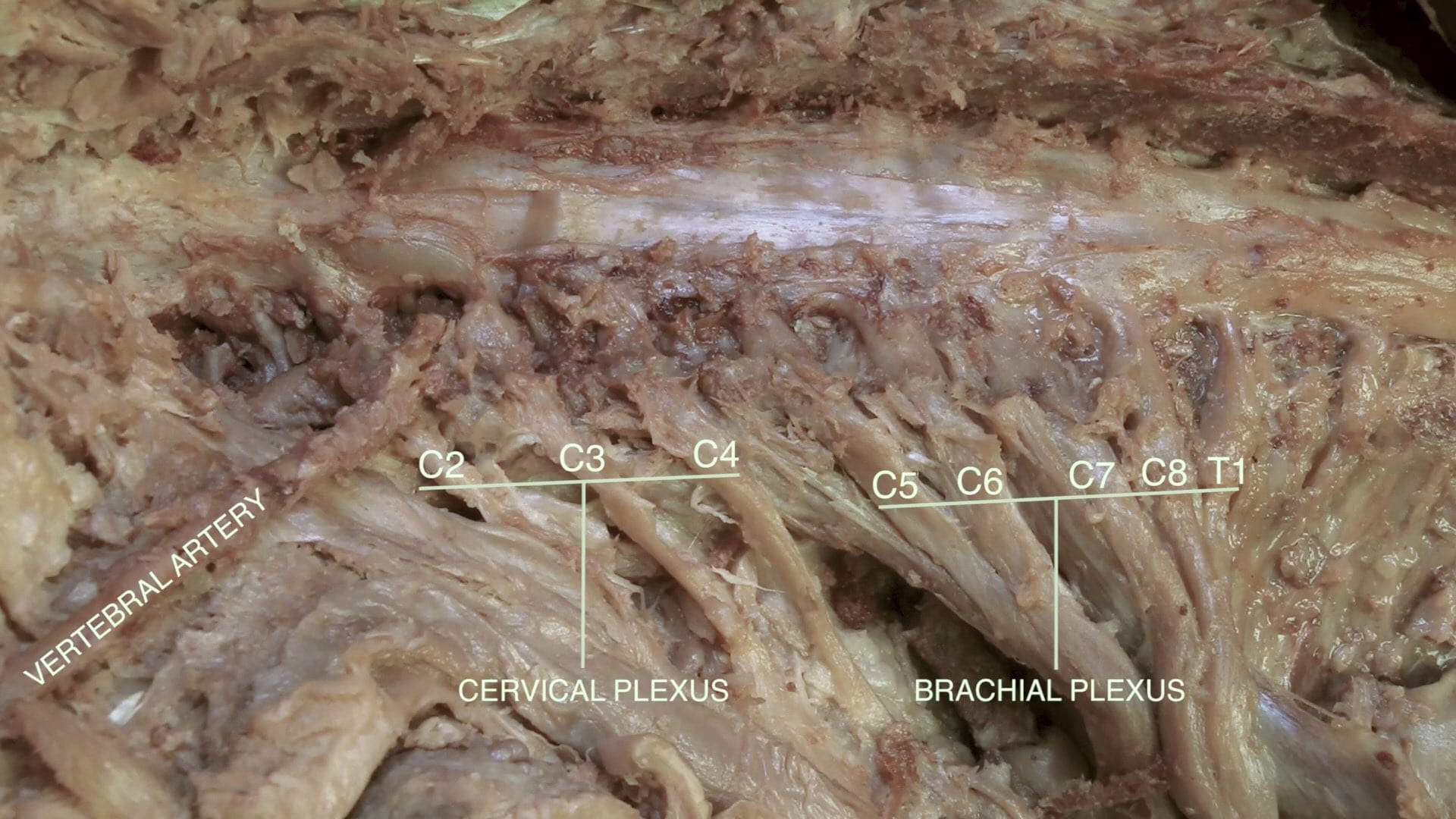
Spine and spinal cord anatomy from foramen magnum to sacrum are taught in this lab. Additionally, this lab includes the posterior dural venous sinuses of the brain, inferior IV ventricle, cervical vertebral artery, cervical, brachial and lumbosacral plexuses.
Lab Objectives
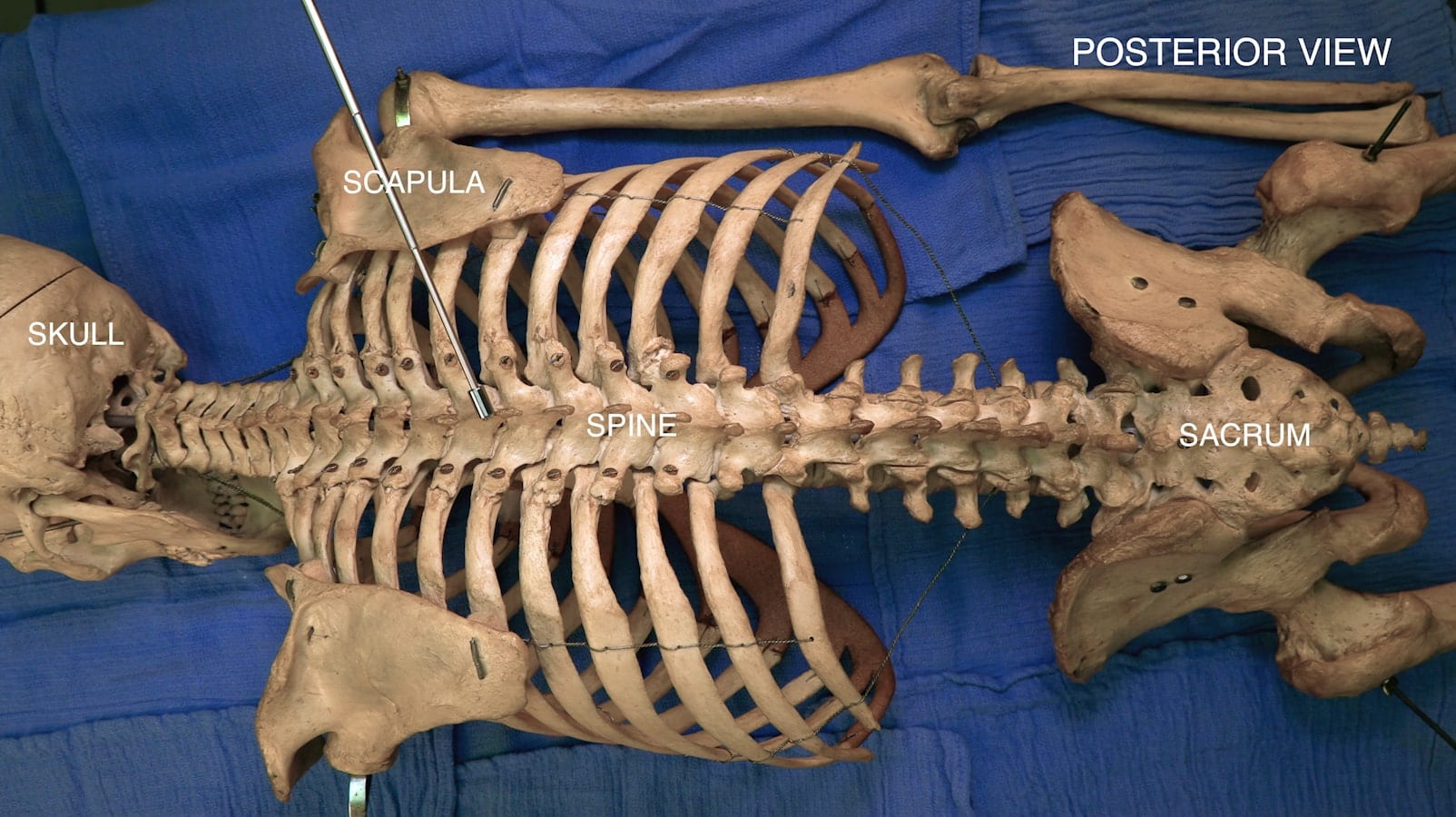
- Describe the vertebral levels of the inferior angle of the scapula and the iliac crest.
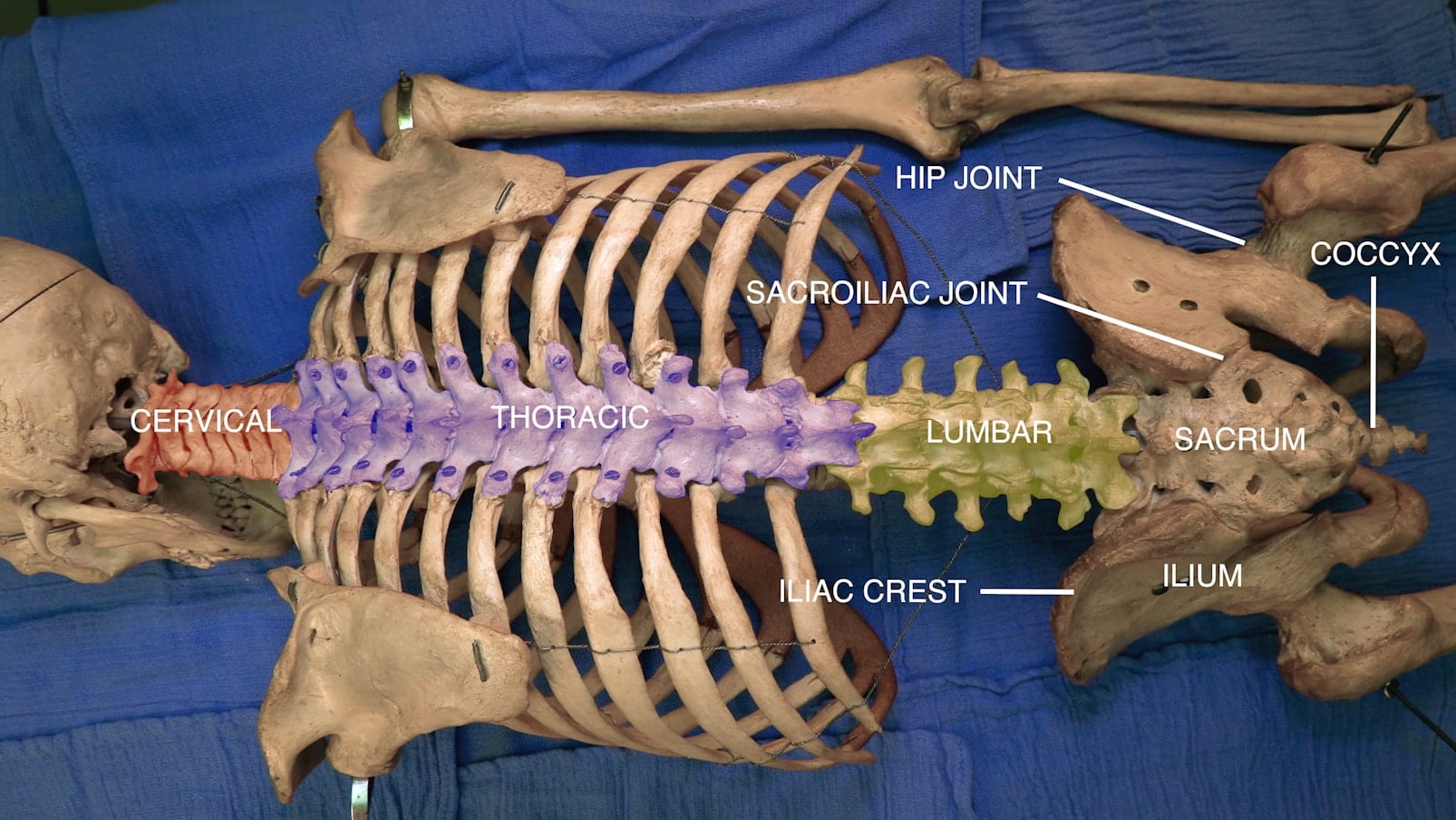
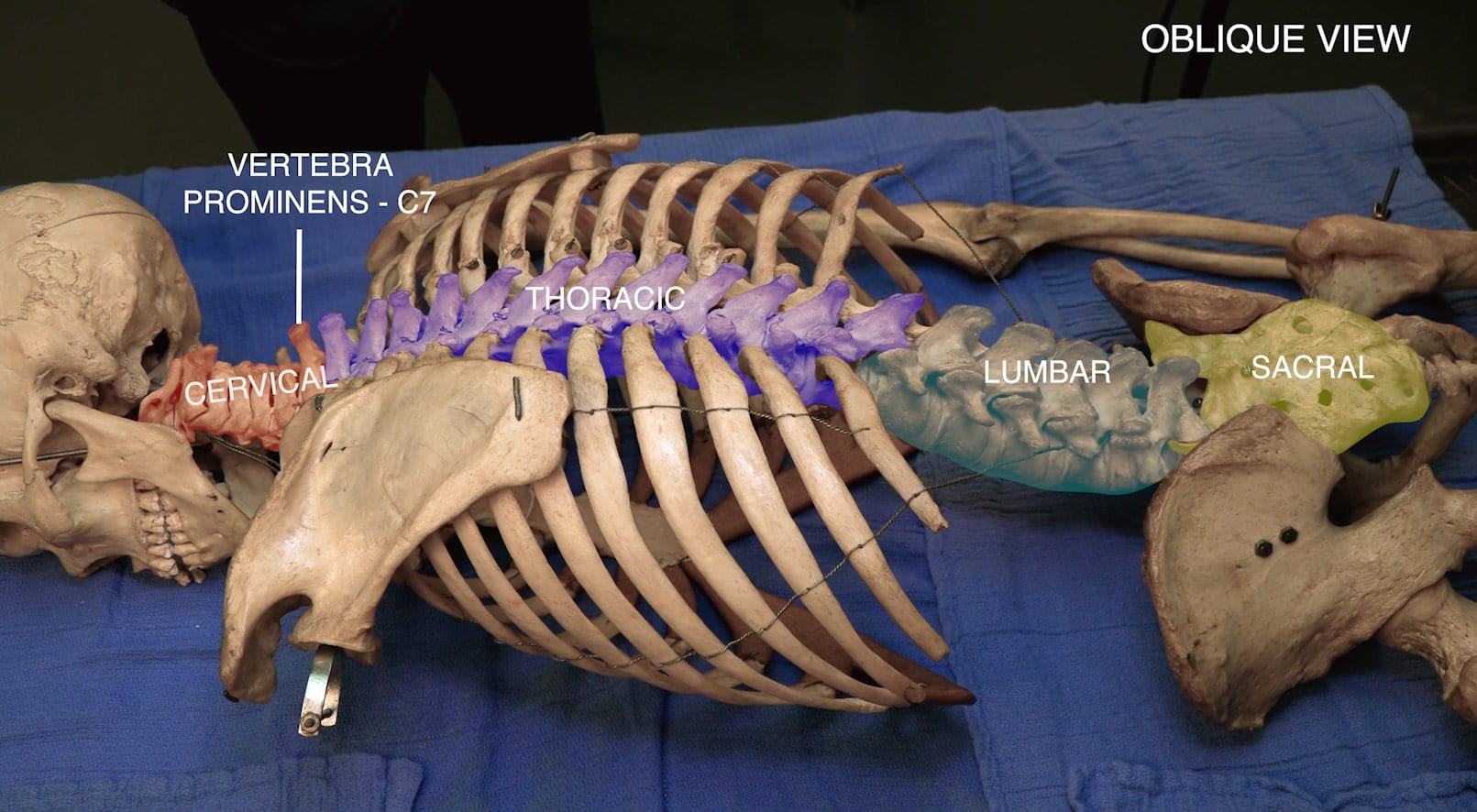
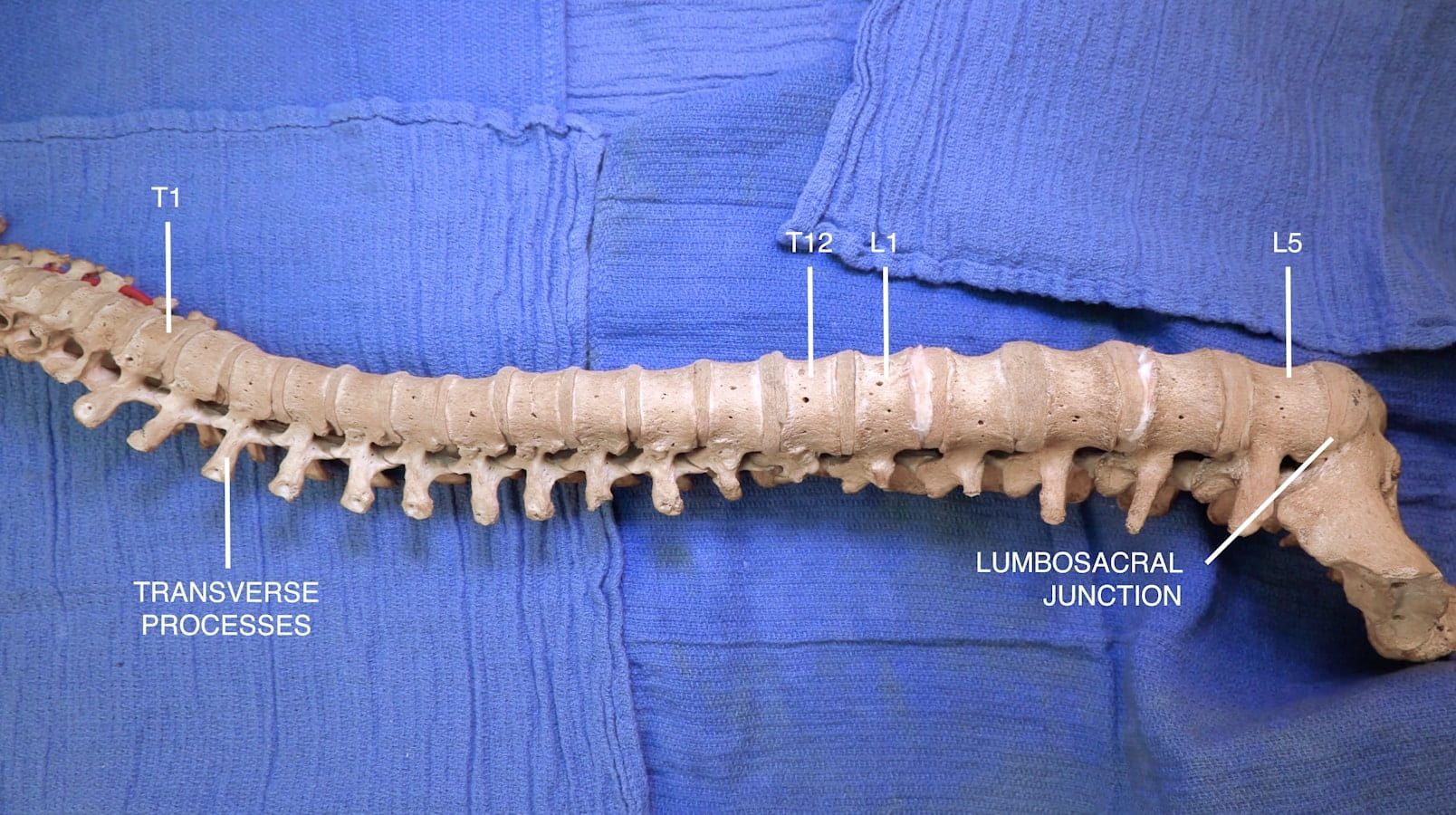
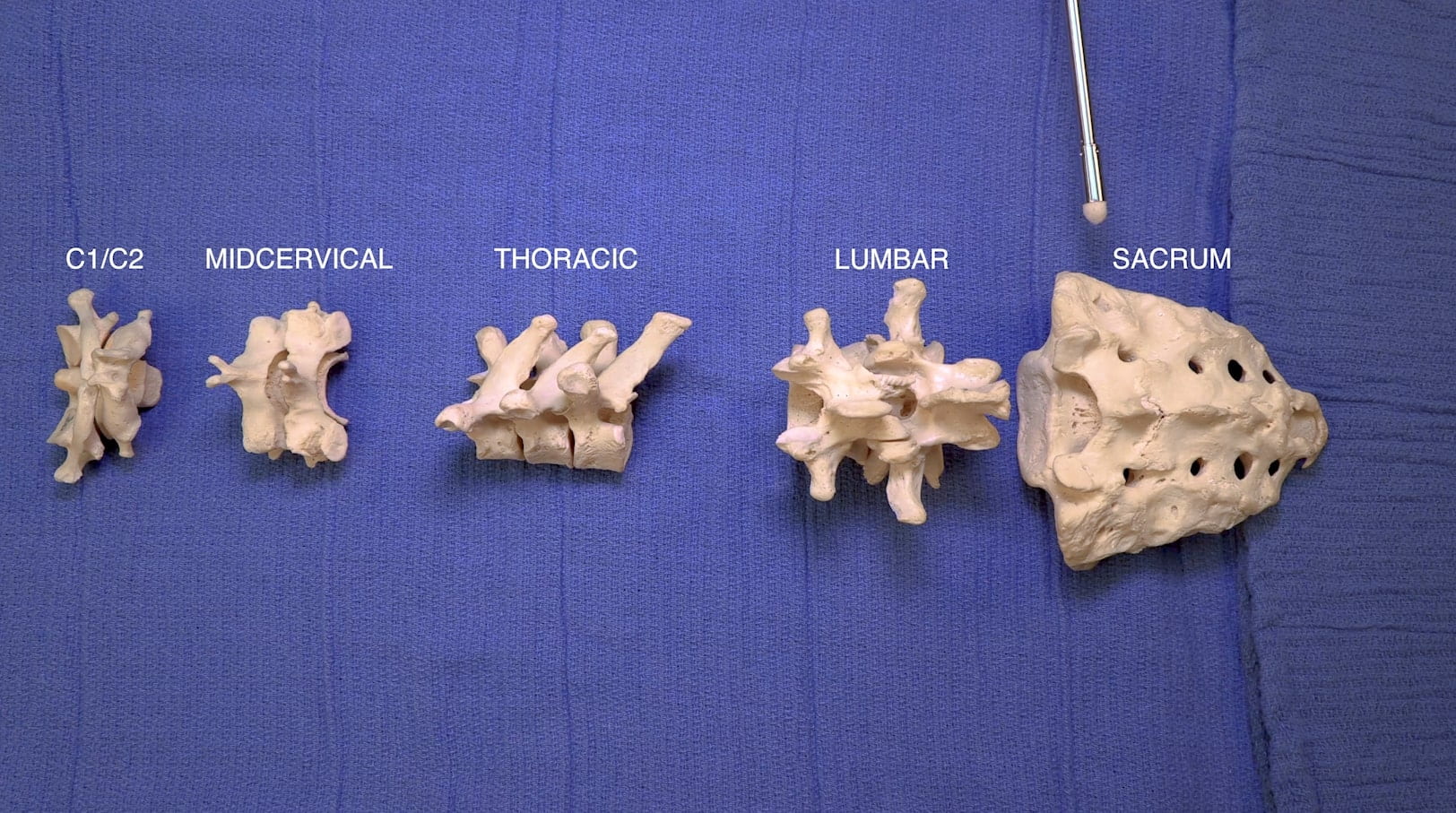
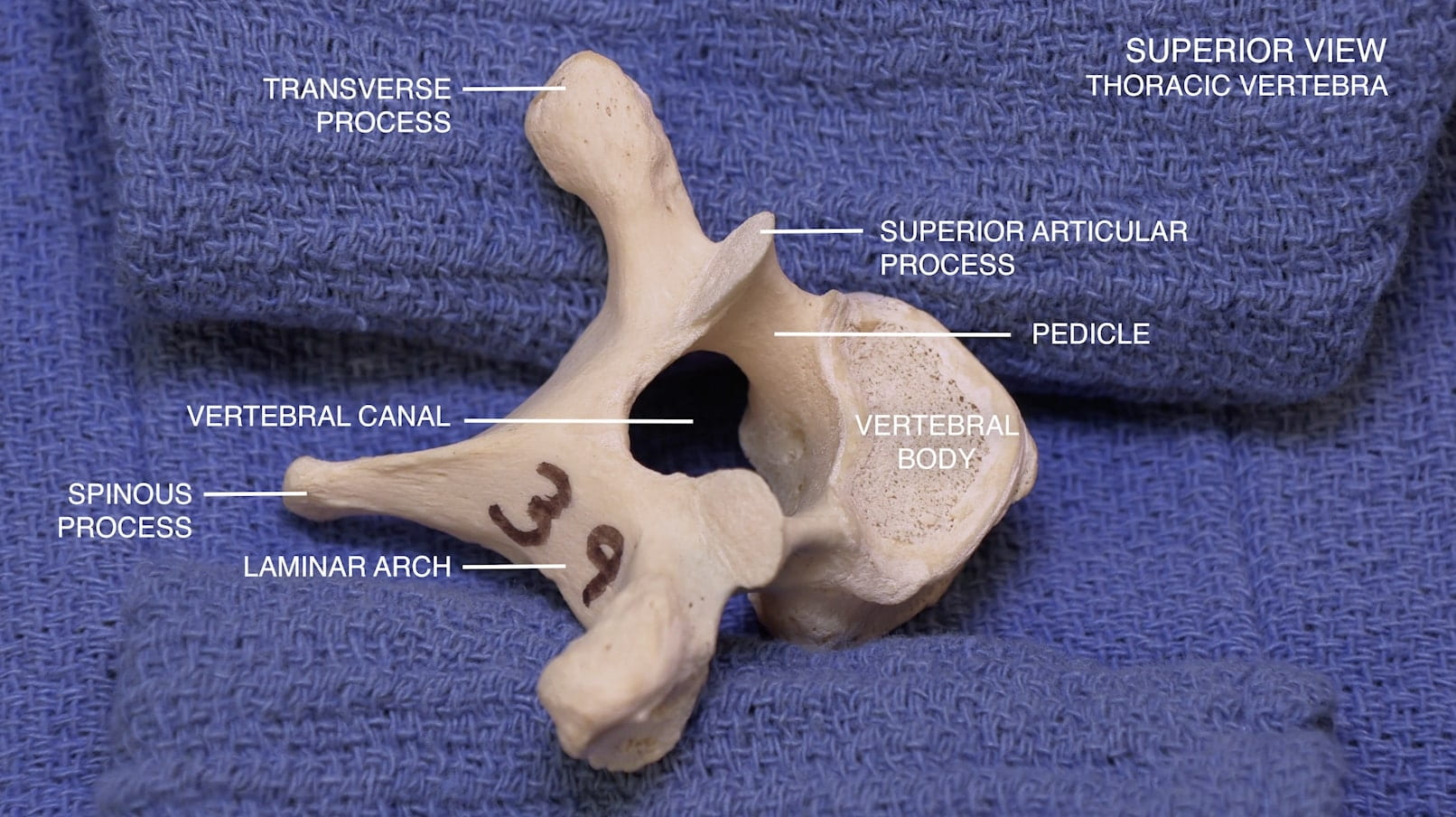
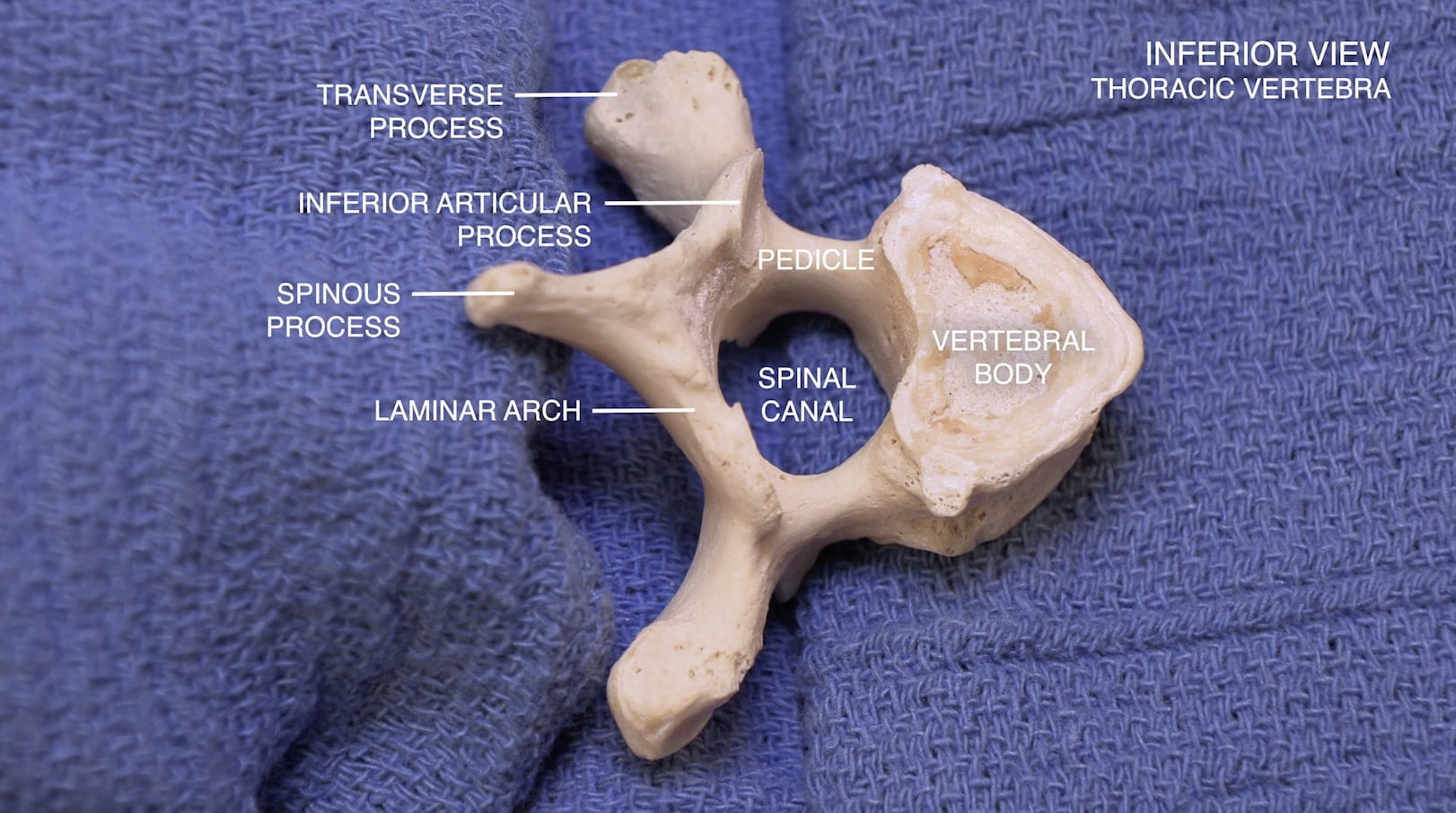
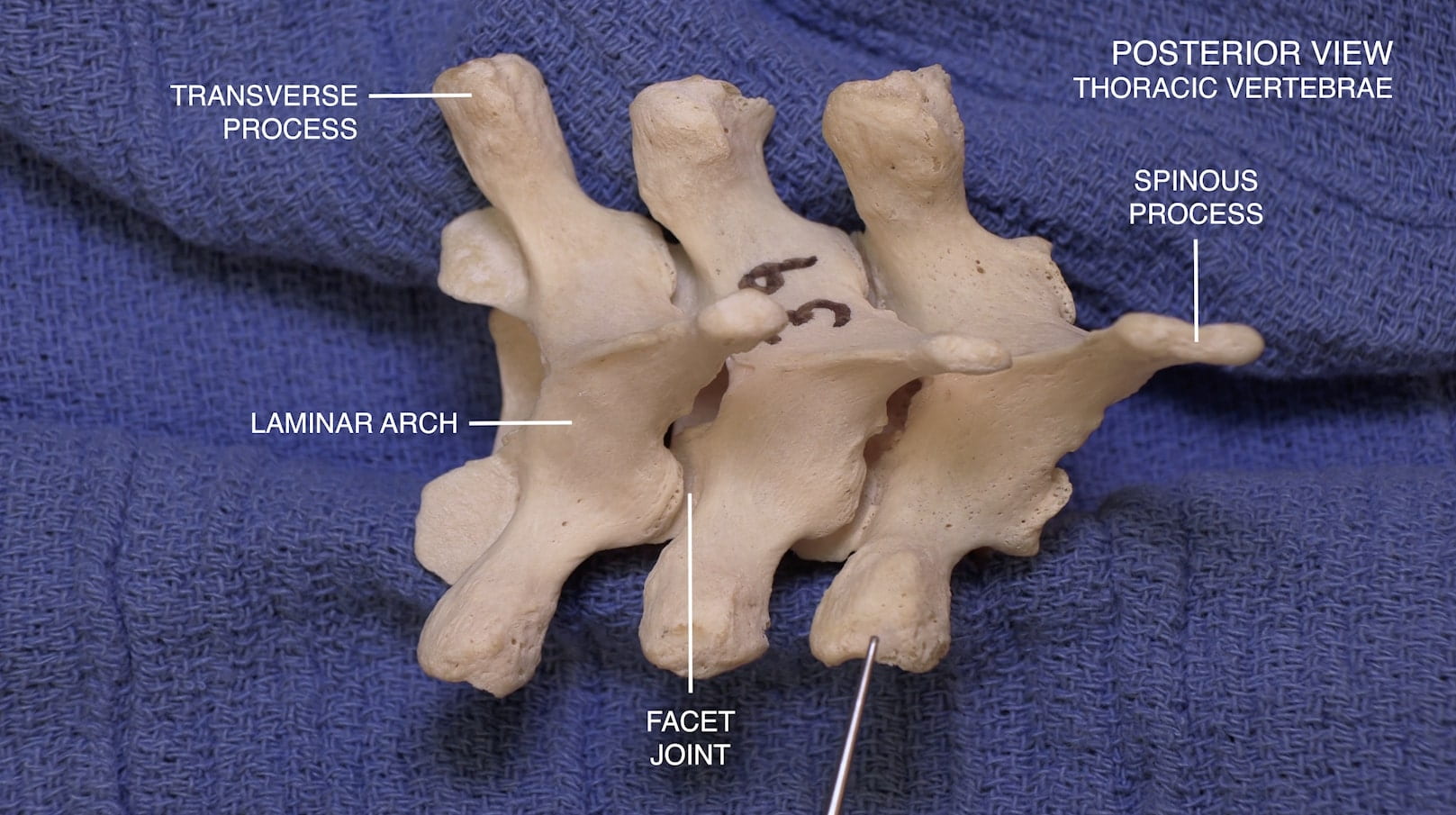
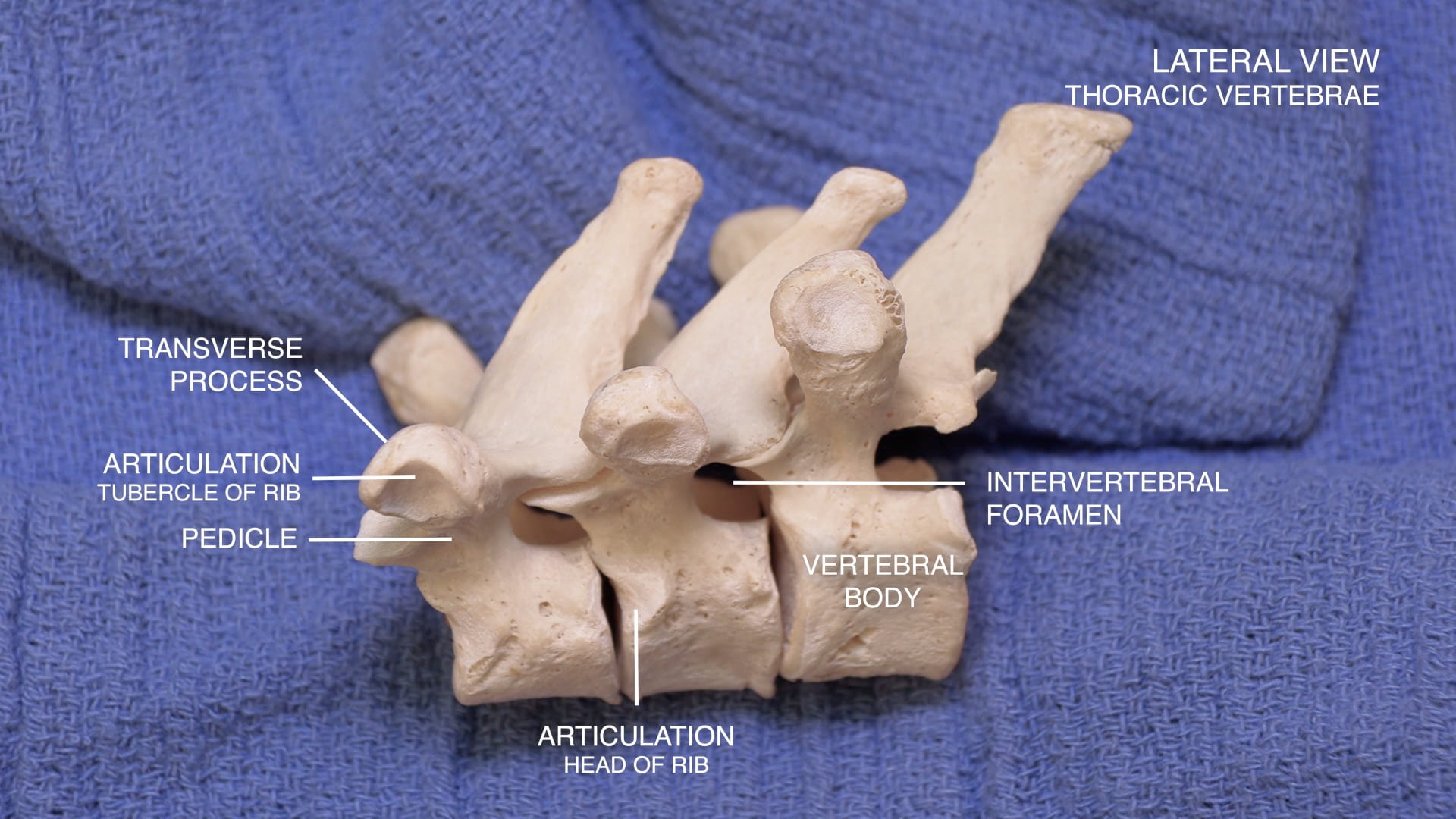
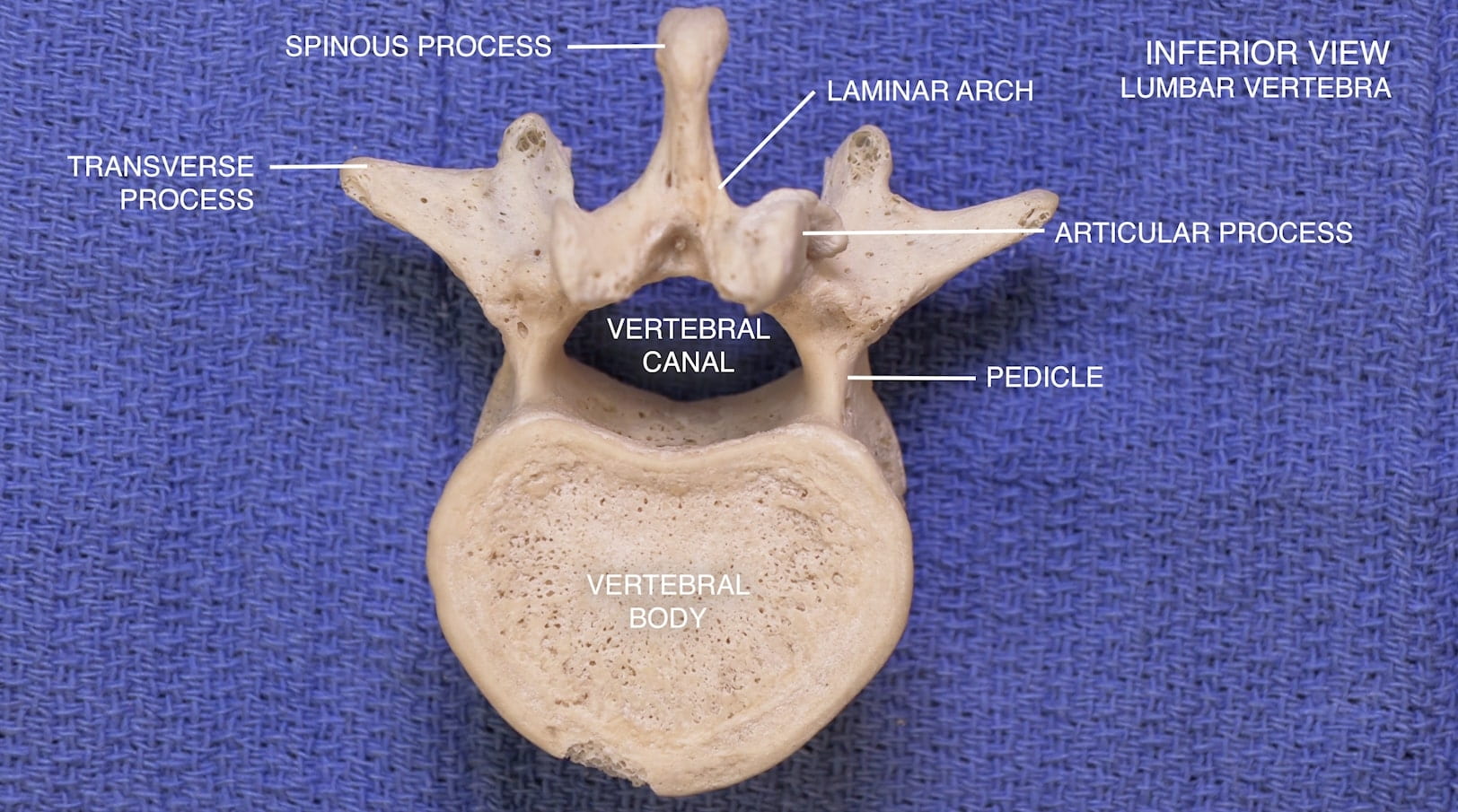
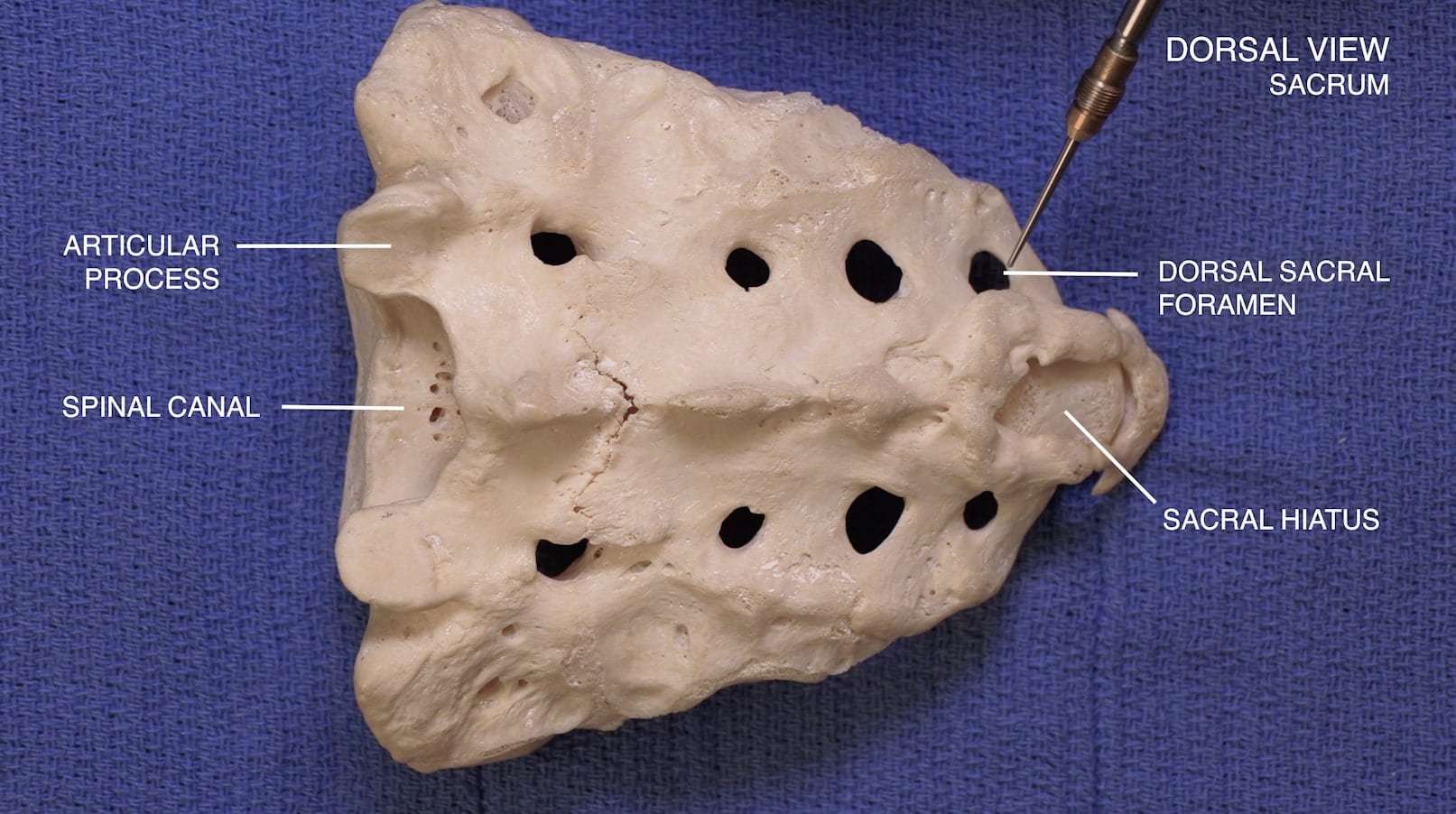
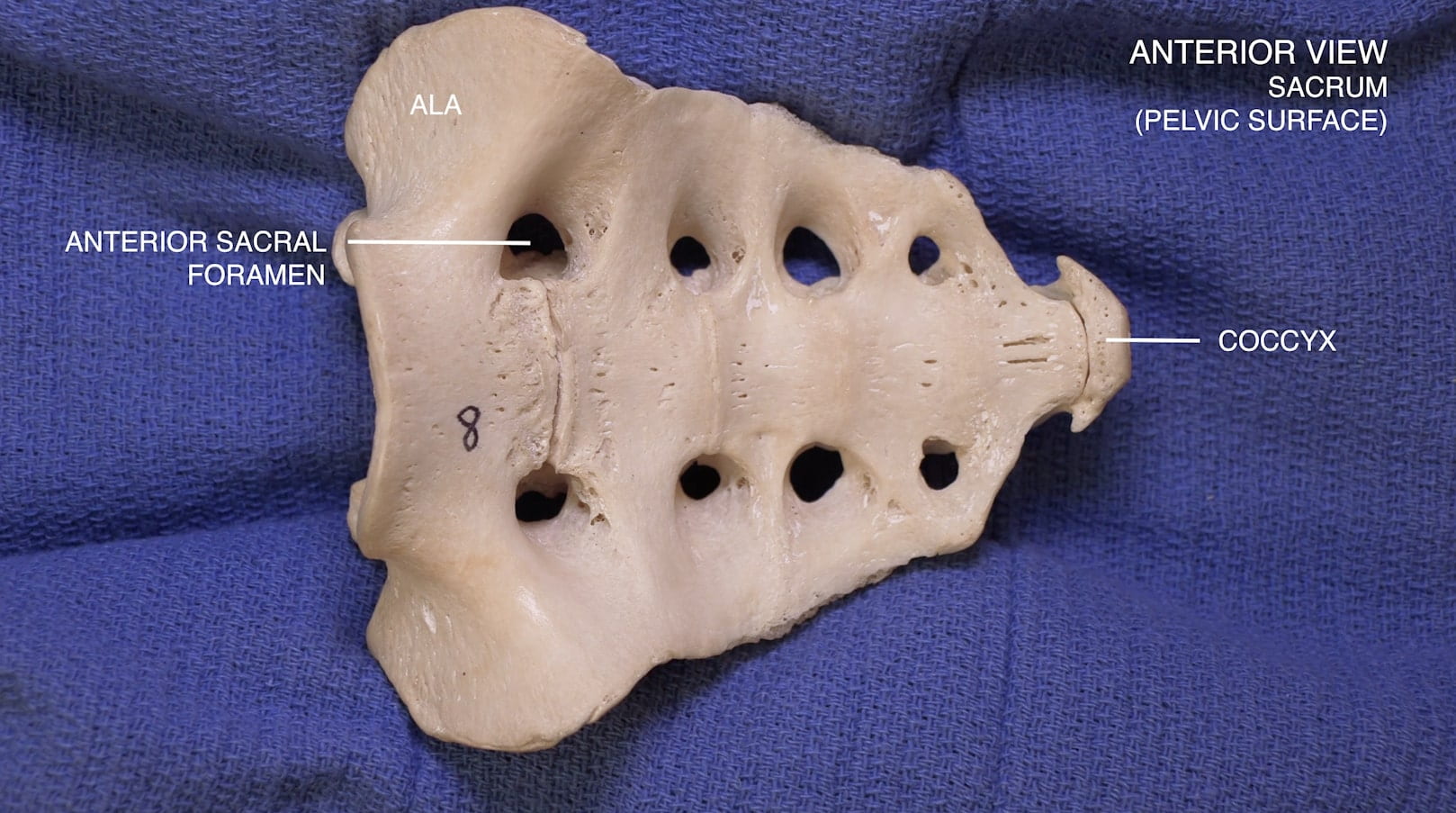
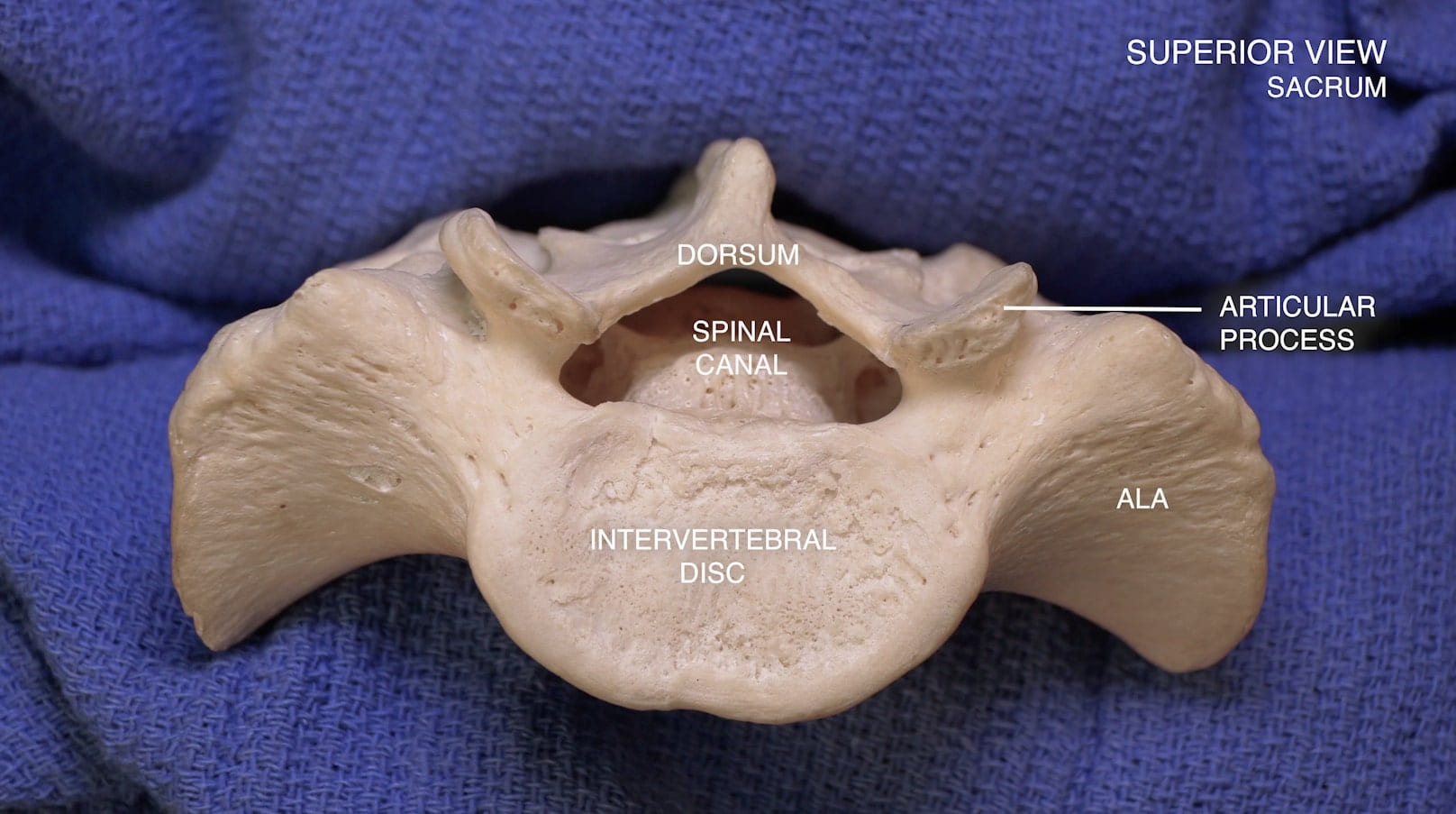
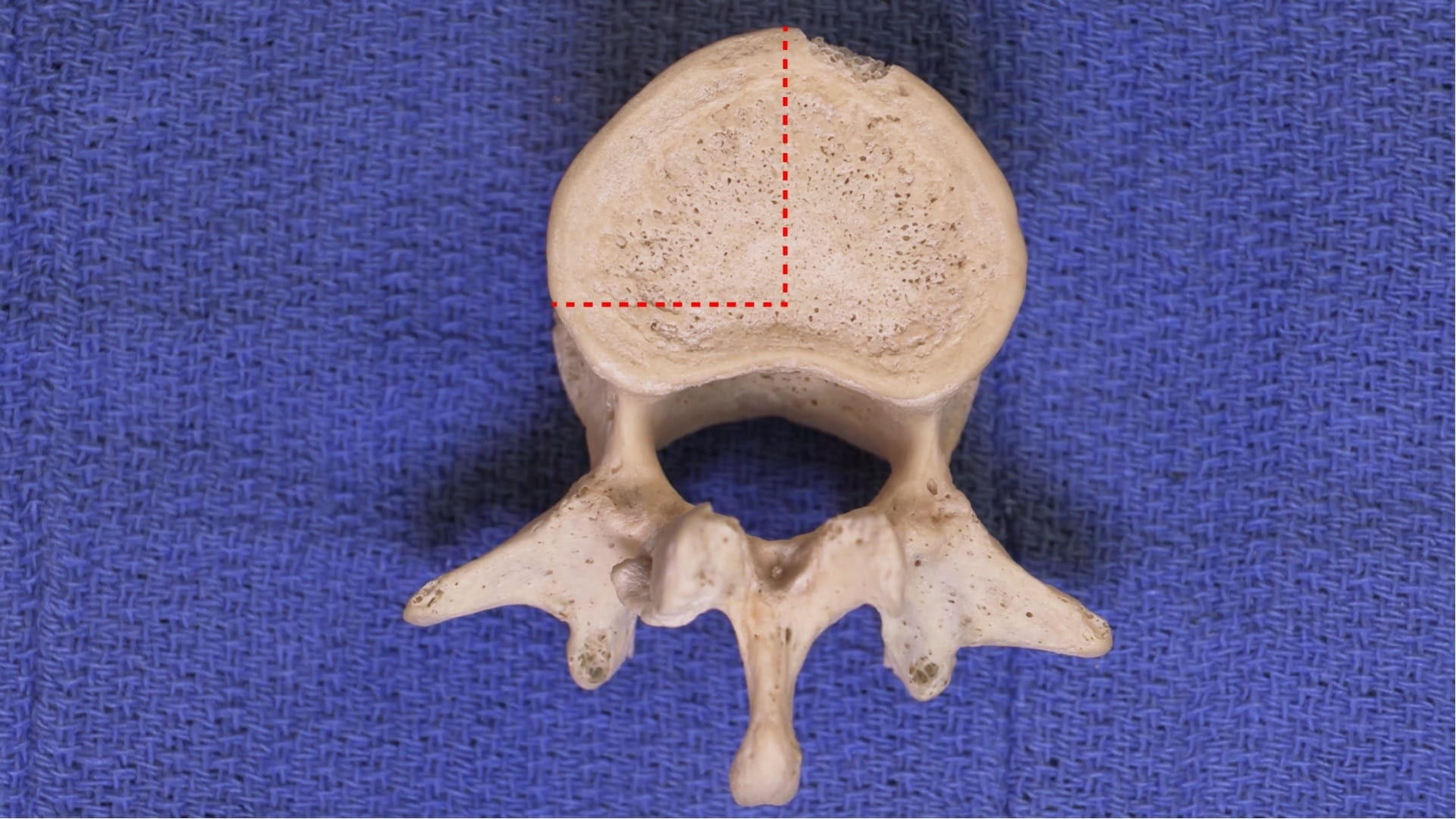
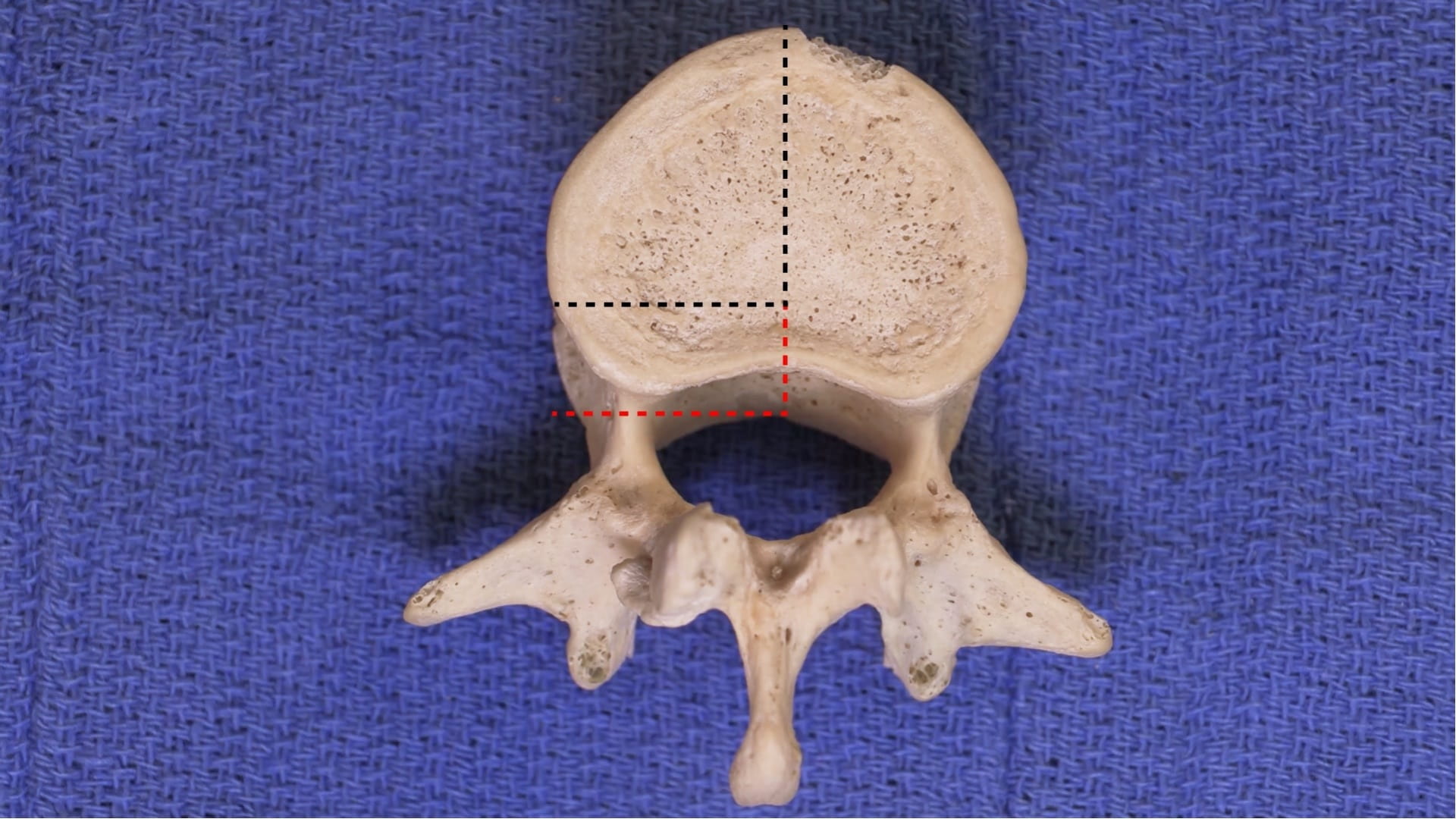
- Describe the features of the cervical, thoracic and lumbar vertebrae and the sacrum.
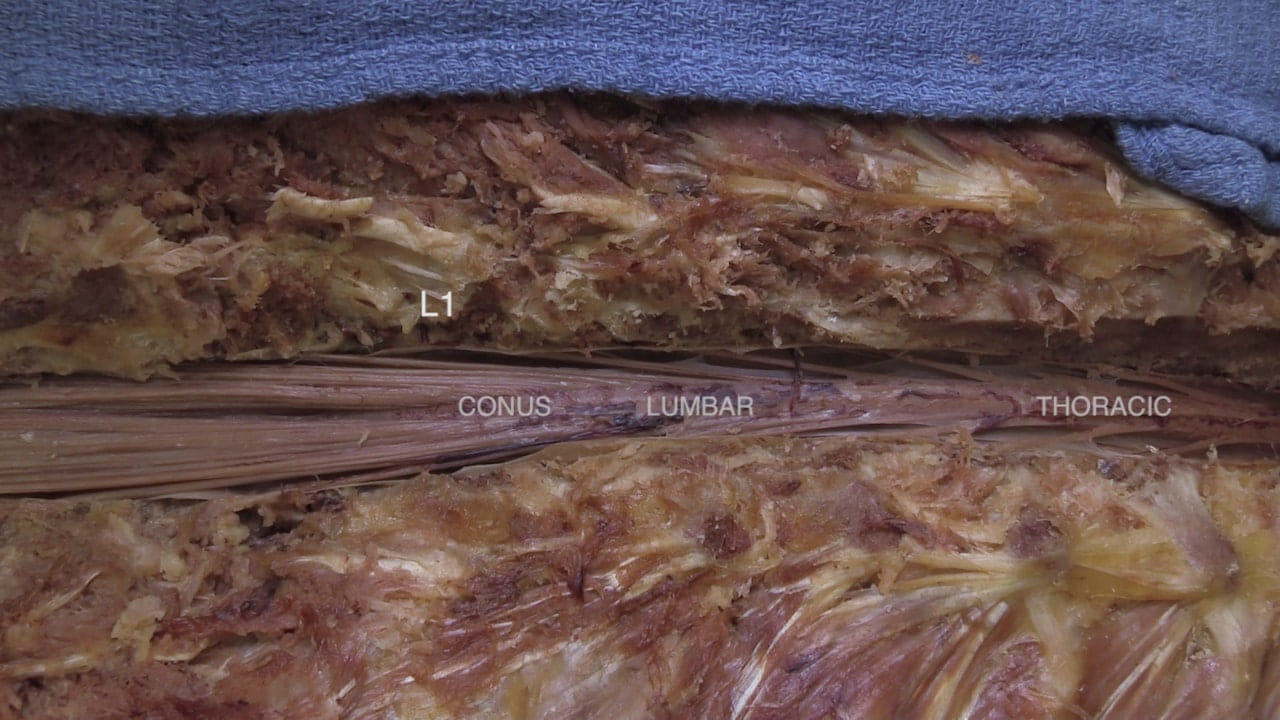
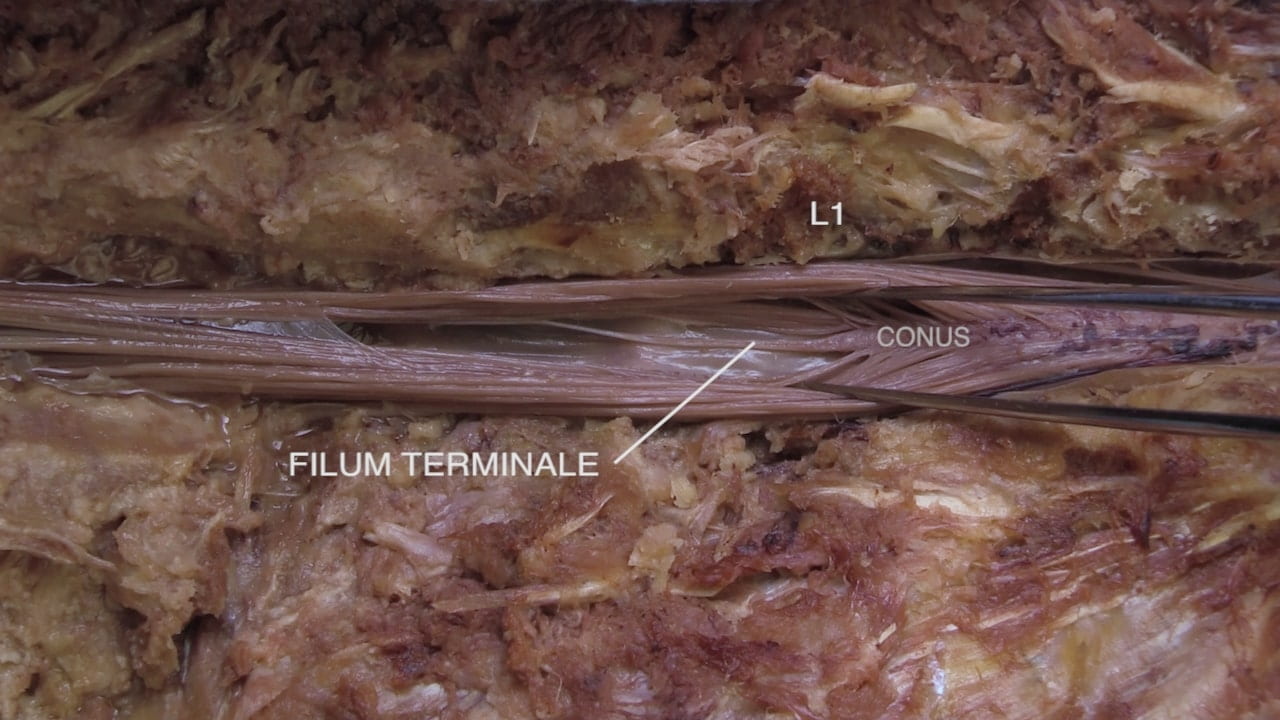
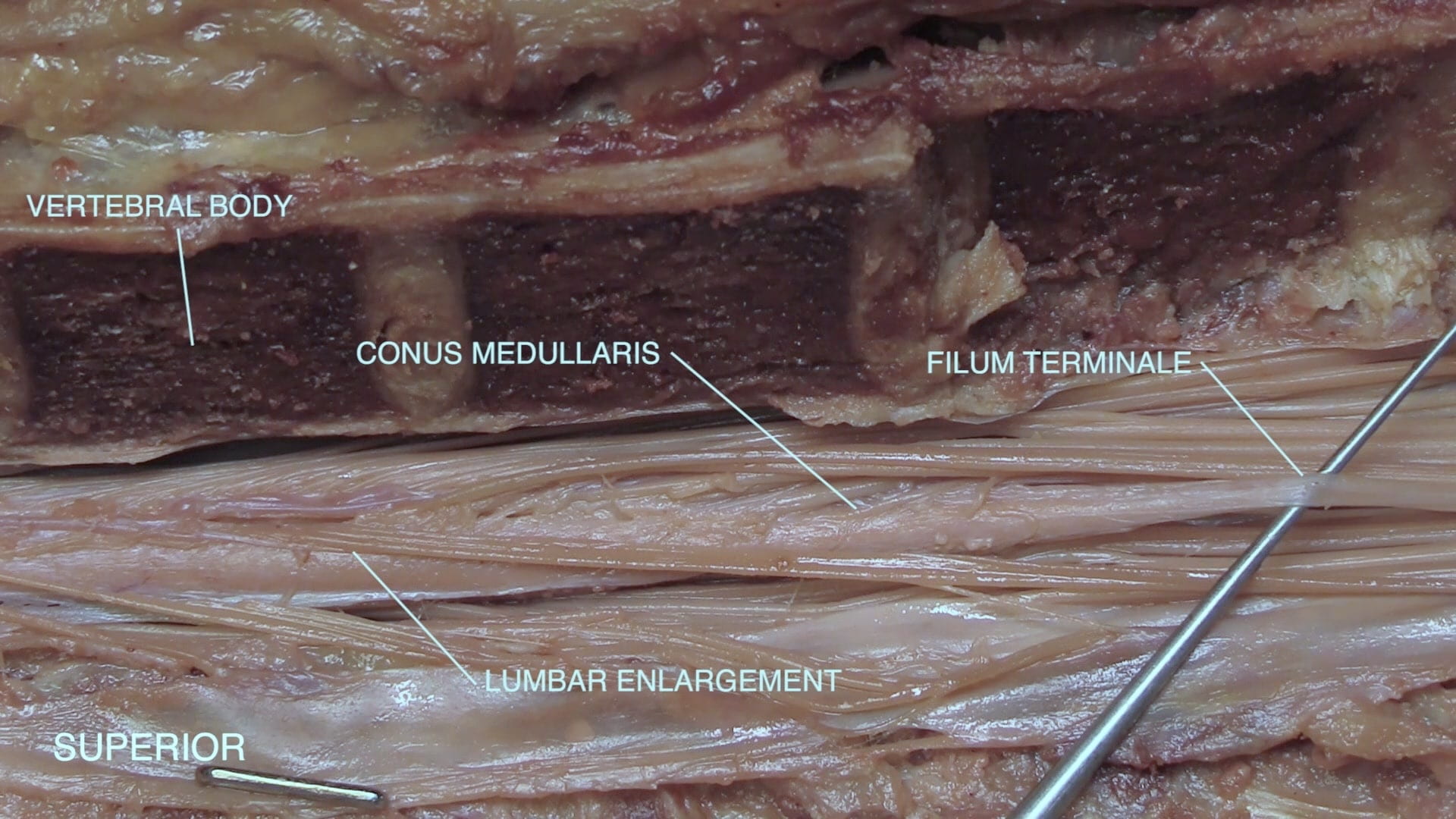
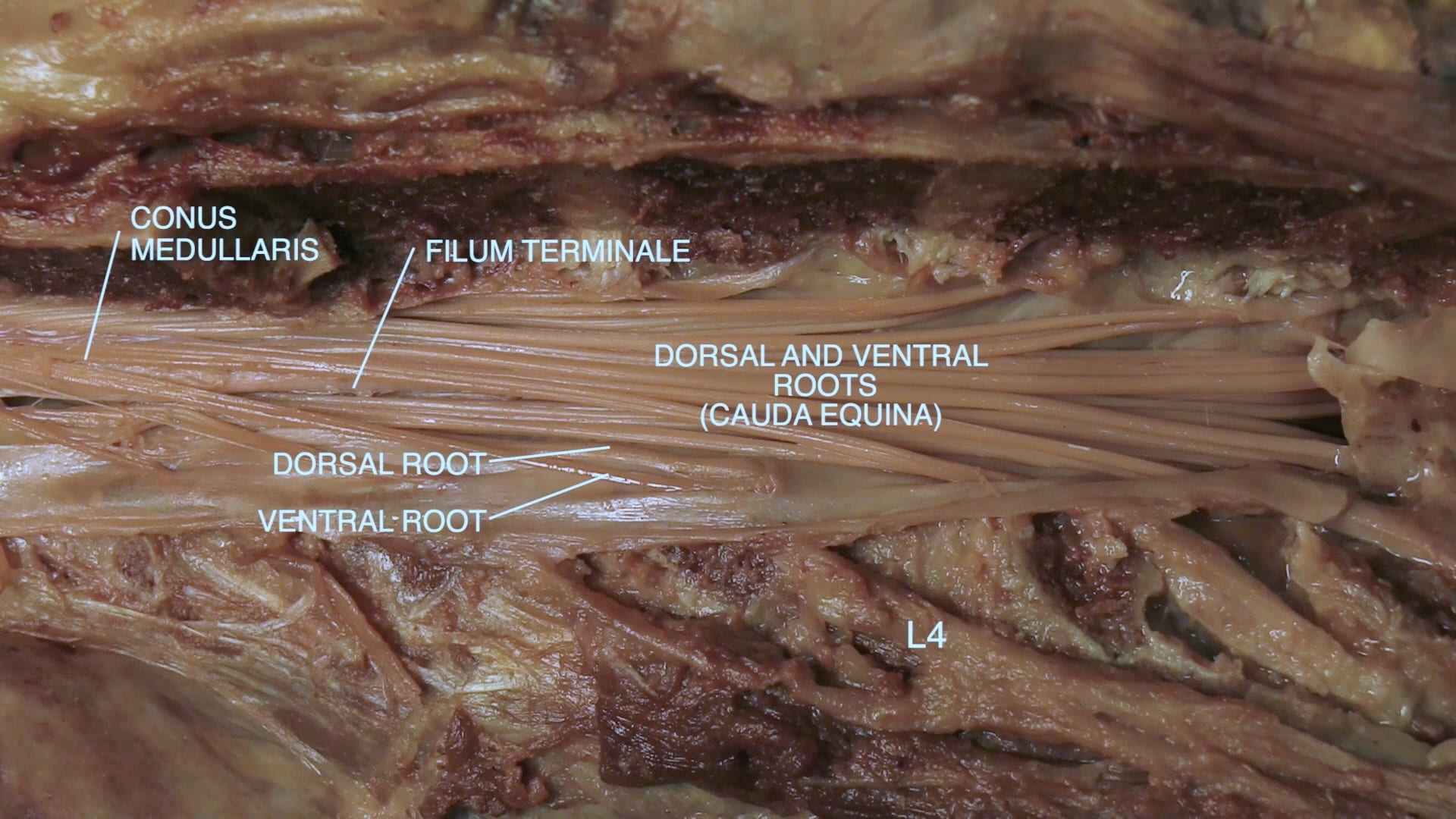
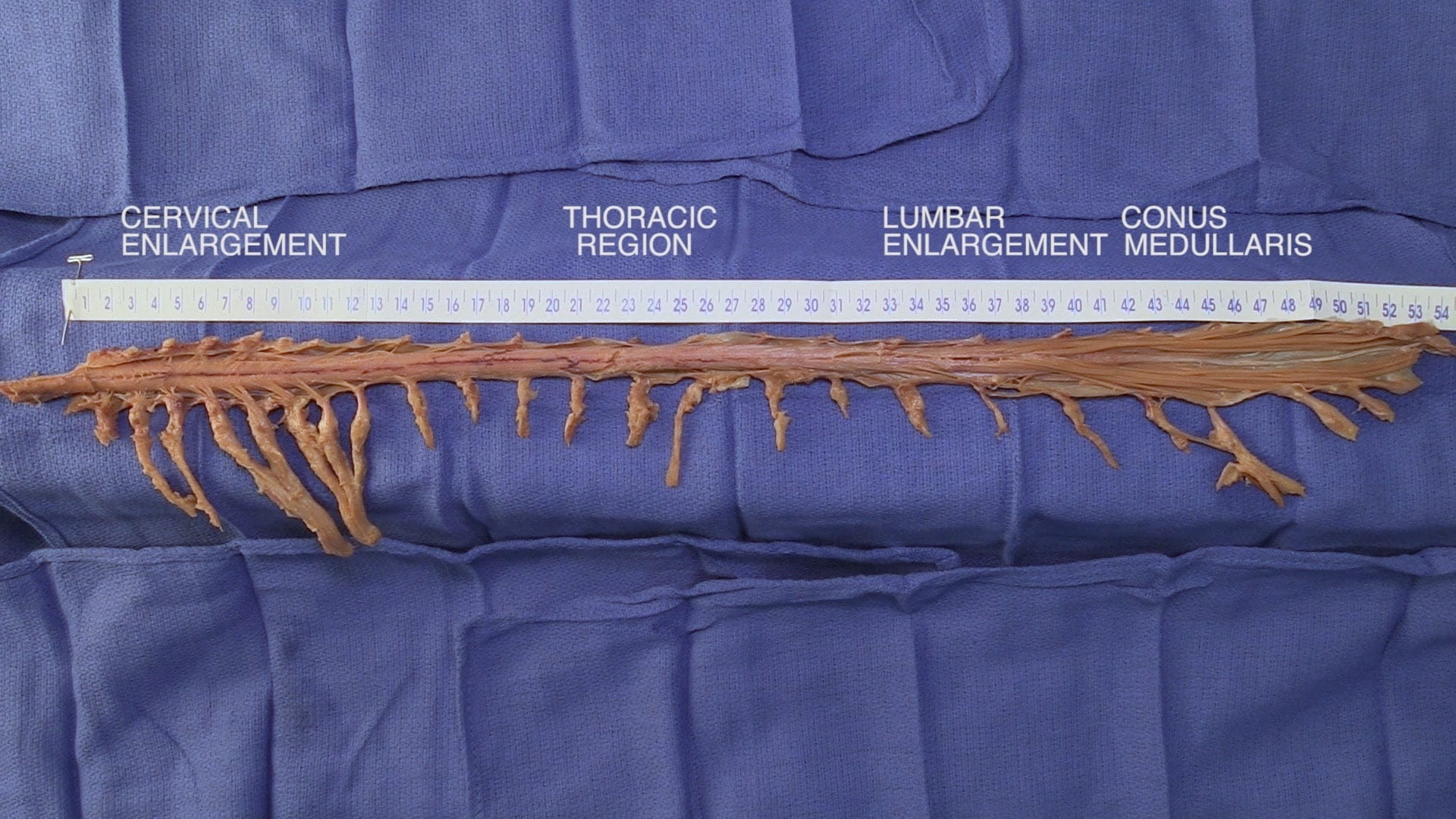
- Describe the vertebral level of the conus medullaris as well as its spinal level.
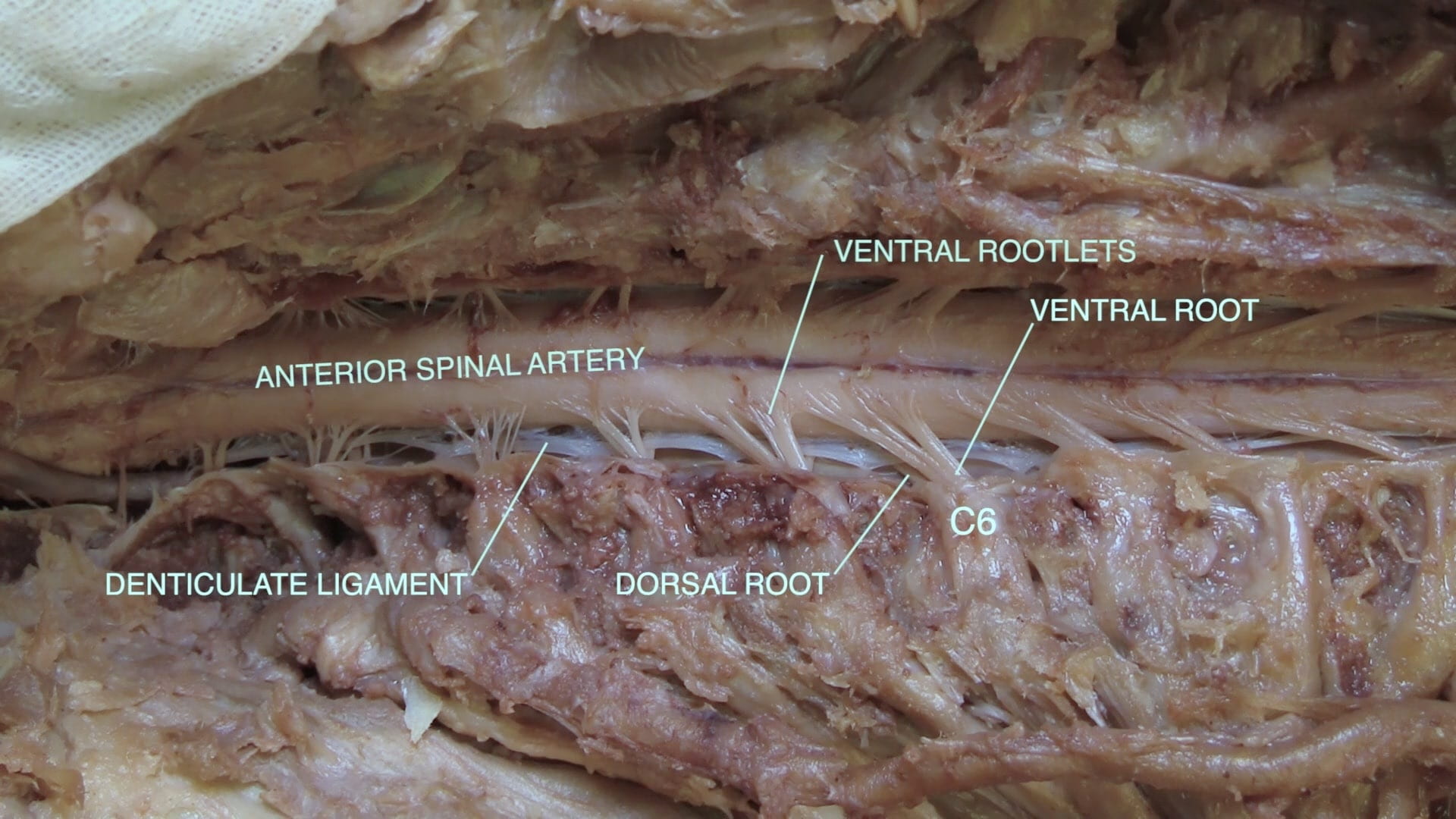
- Describe the blood supply of the spinal cord.
- Describe the best site to perform a lumbar puncture.
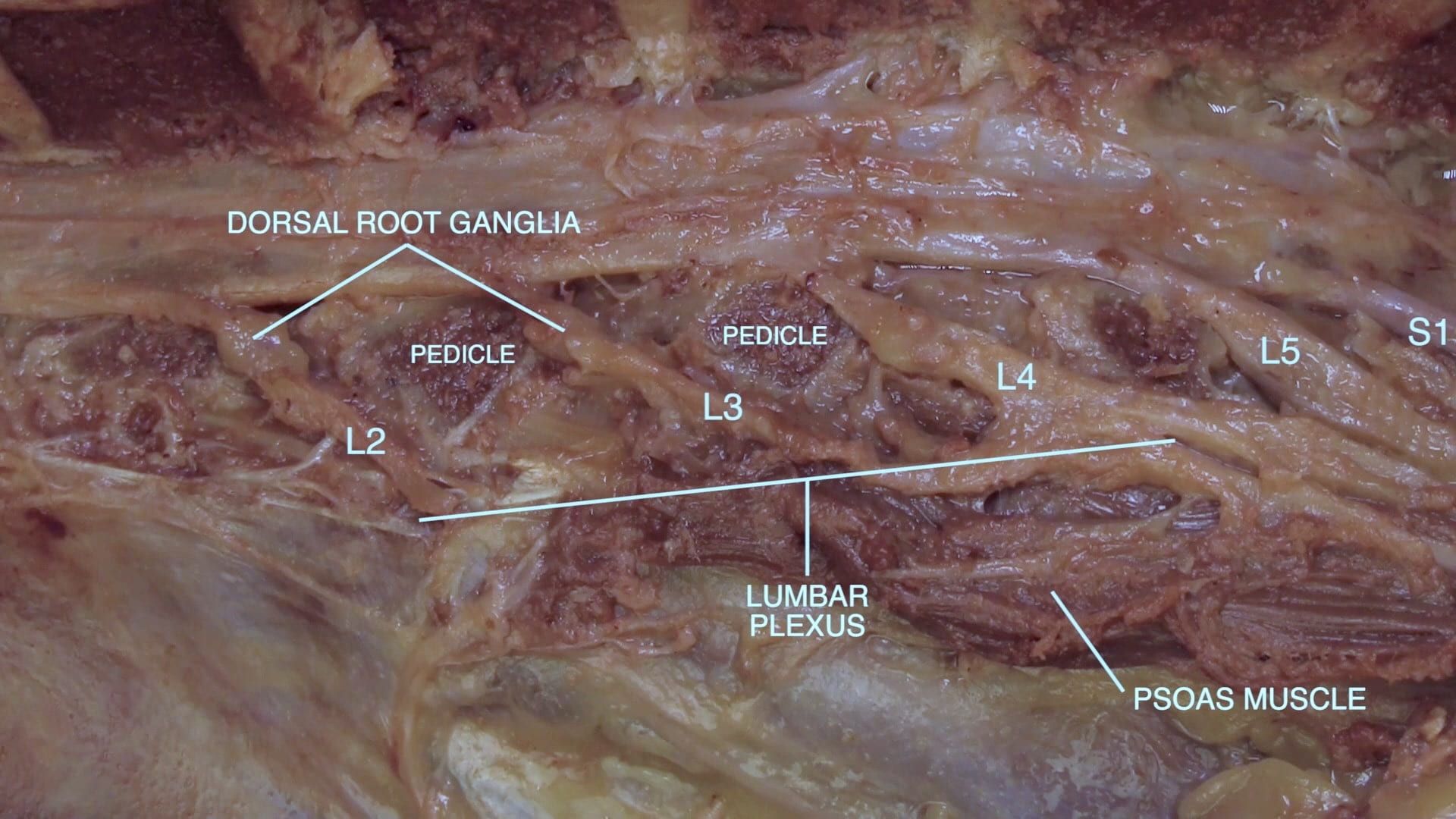
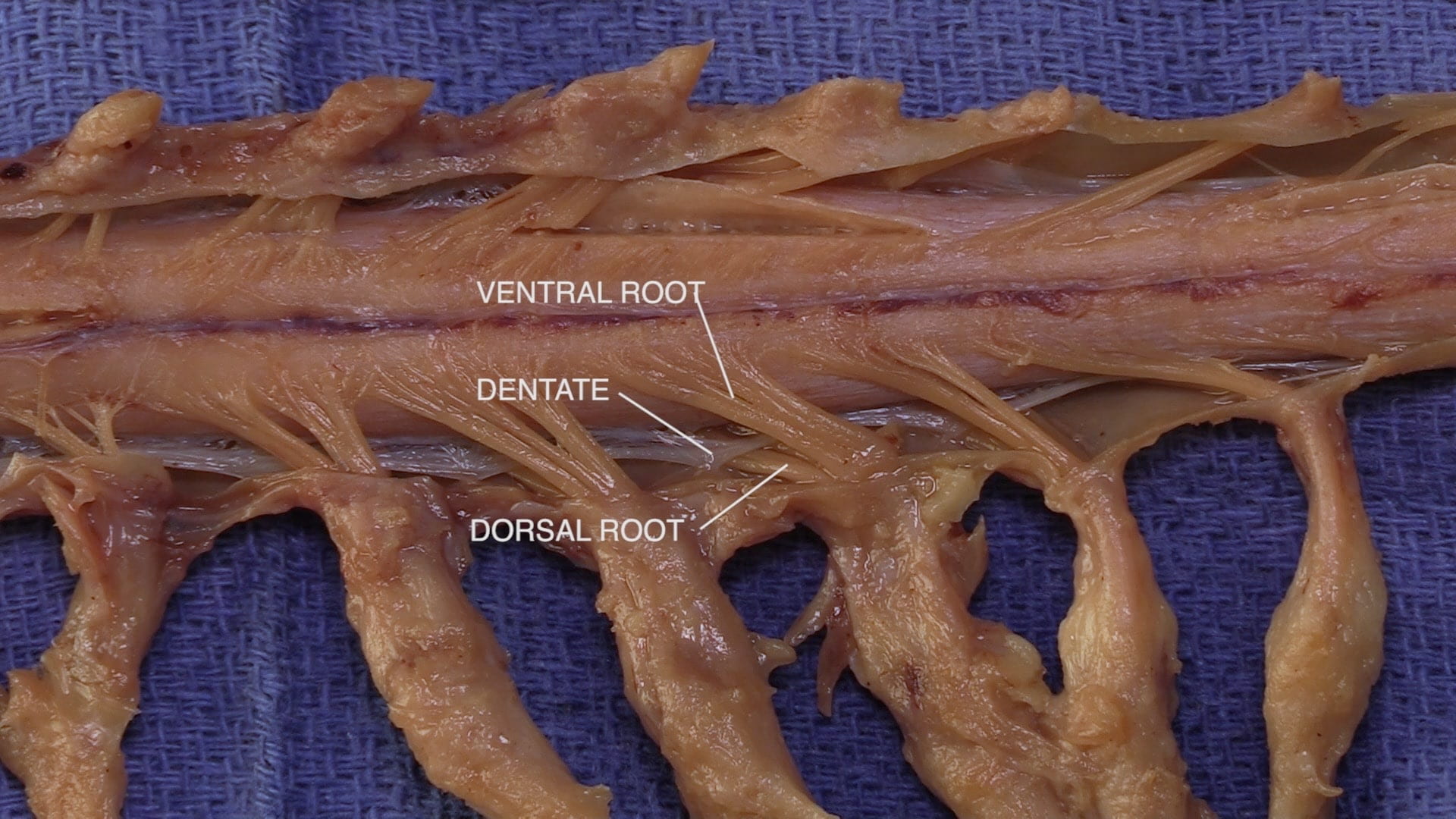
- Describe the formation of a spinal nerve.
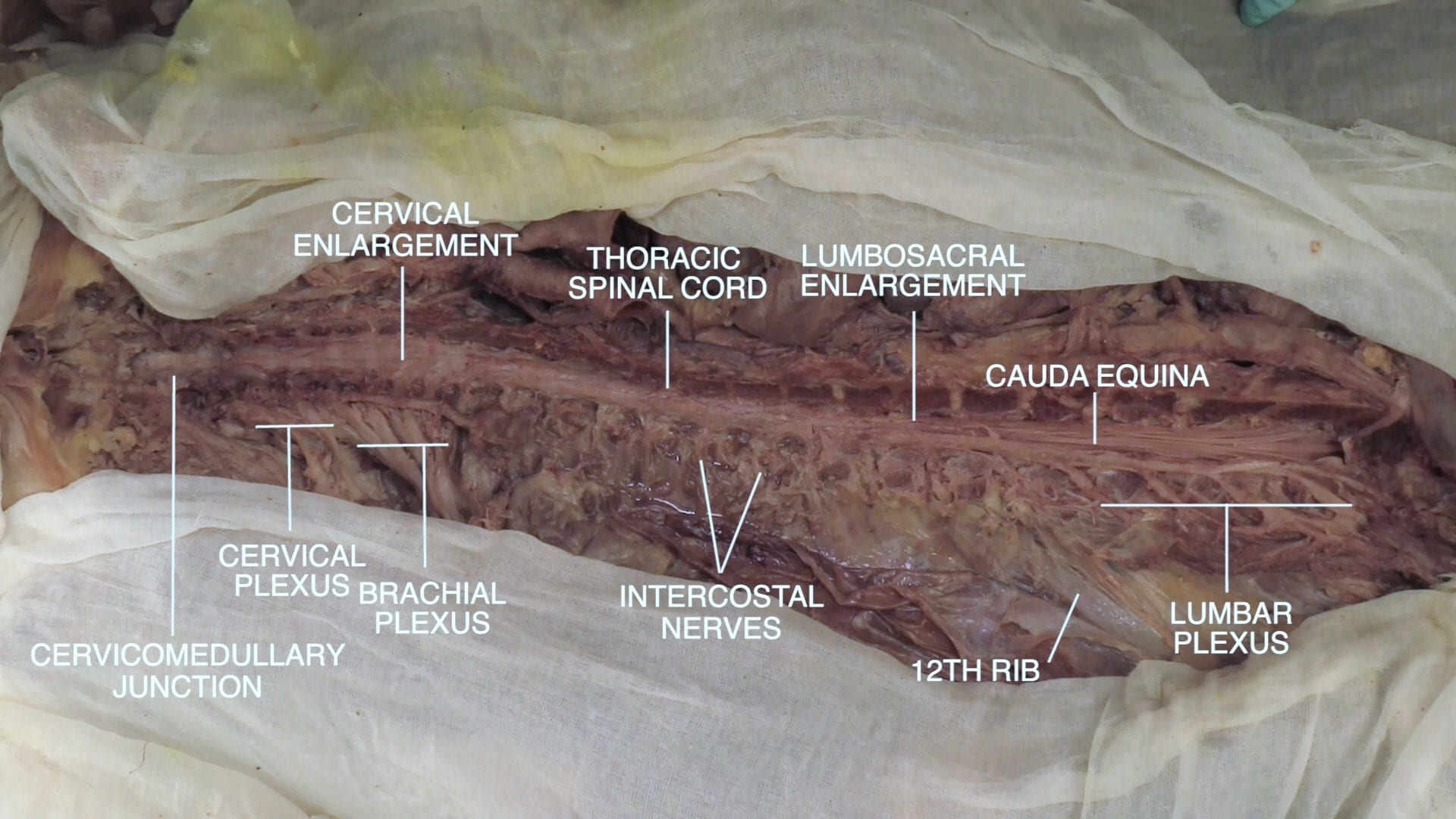
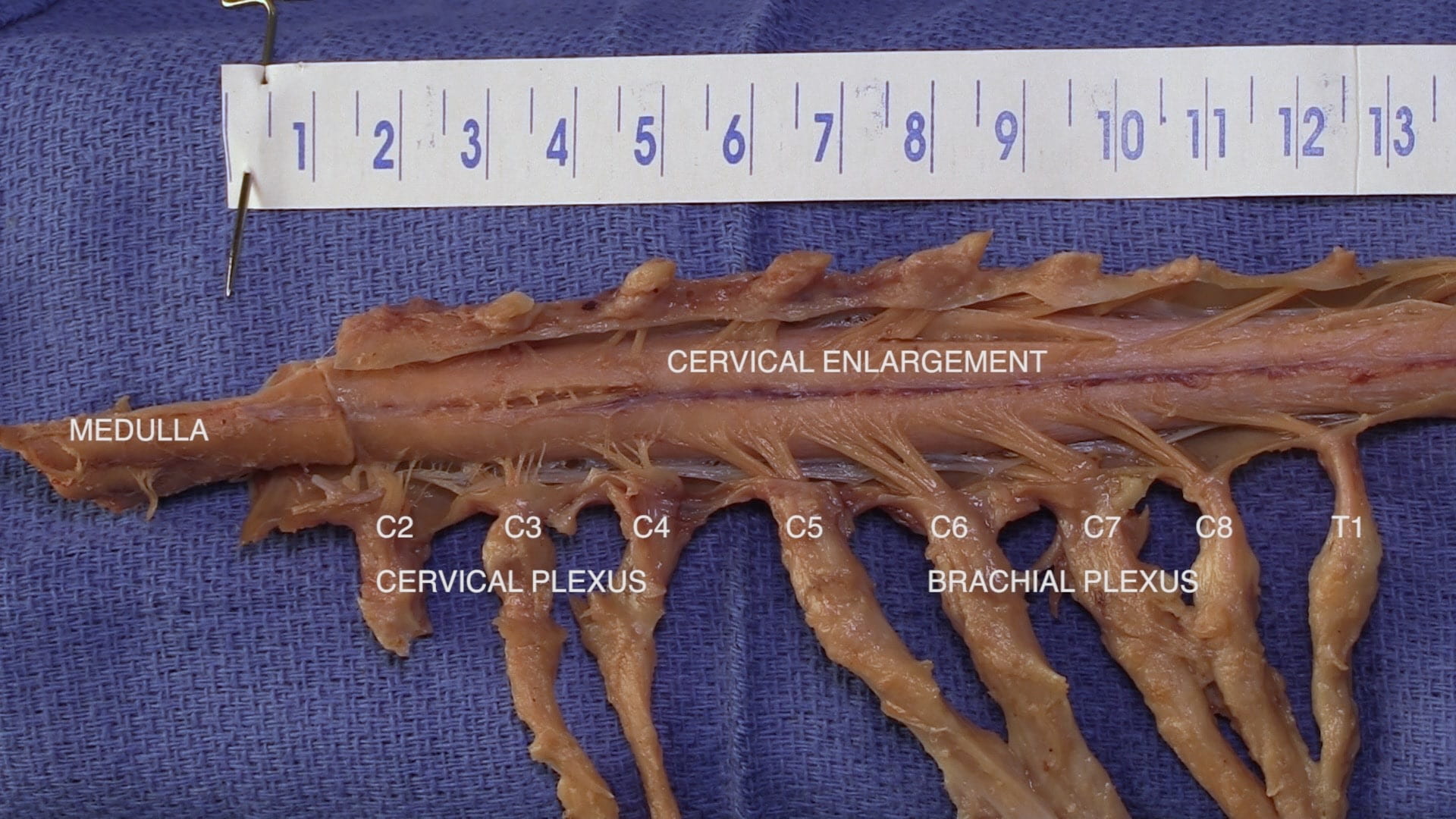
- Describe the significance of the cervical enlargement of the spinal cord.
- Name the spinal levels of the cervical plexus, brachial plexus and lumbar plexus.
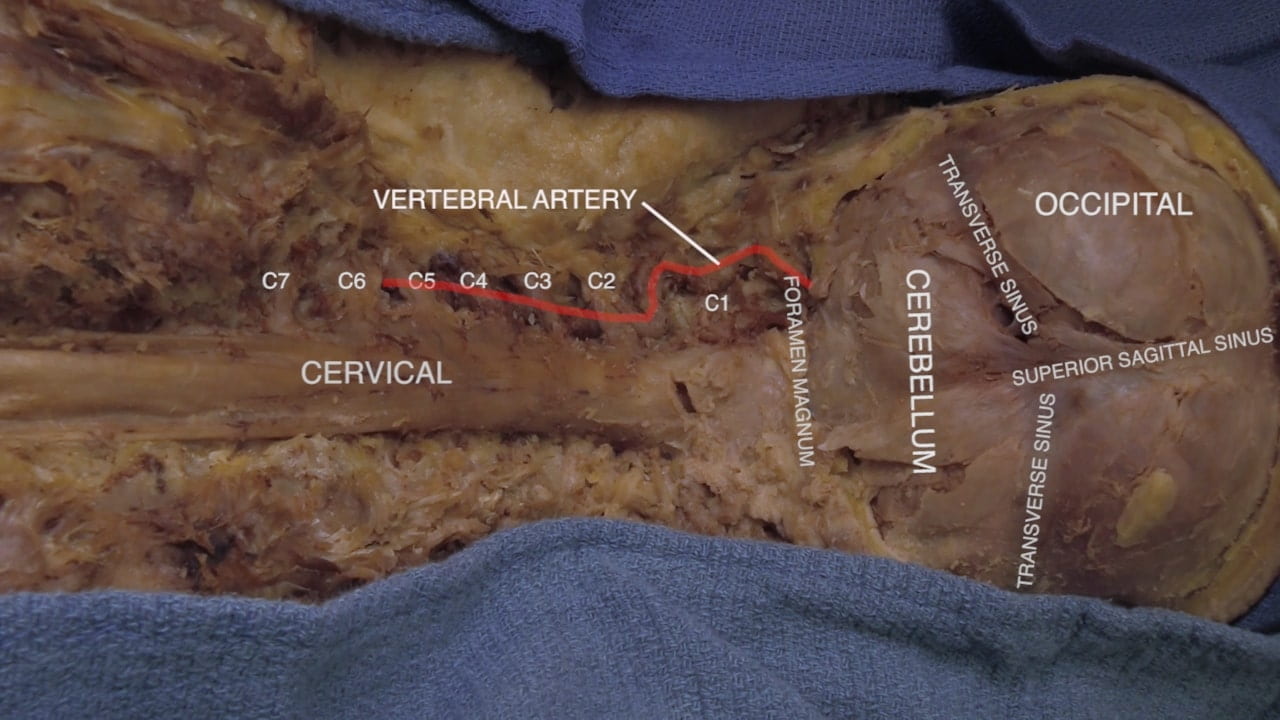
- Describe the course of the vertebral arteries and their contribution to the brain and spinal cord circulation.
Lecture List
Spinal Column Part I & II, Exposure of the Posterior Spine and Spinal Canal, Dorsal Brain and Spinal Cord, Expose Ventral Spinal Cord, Ventral Spinal Cord, Removed Spinal Cord
Spinal Column Part I
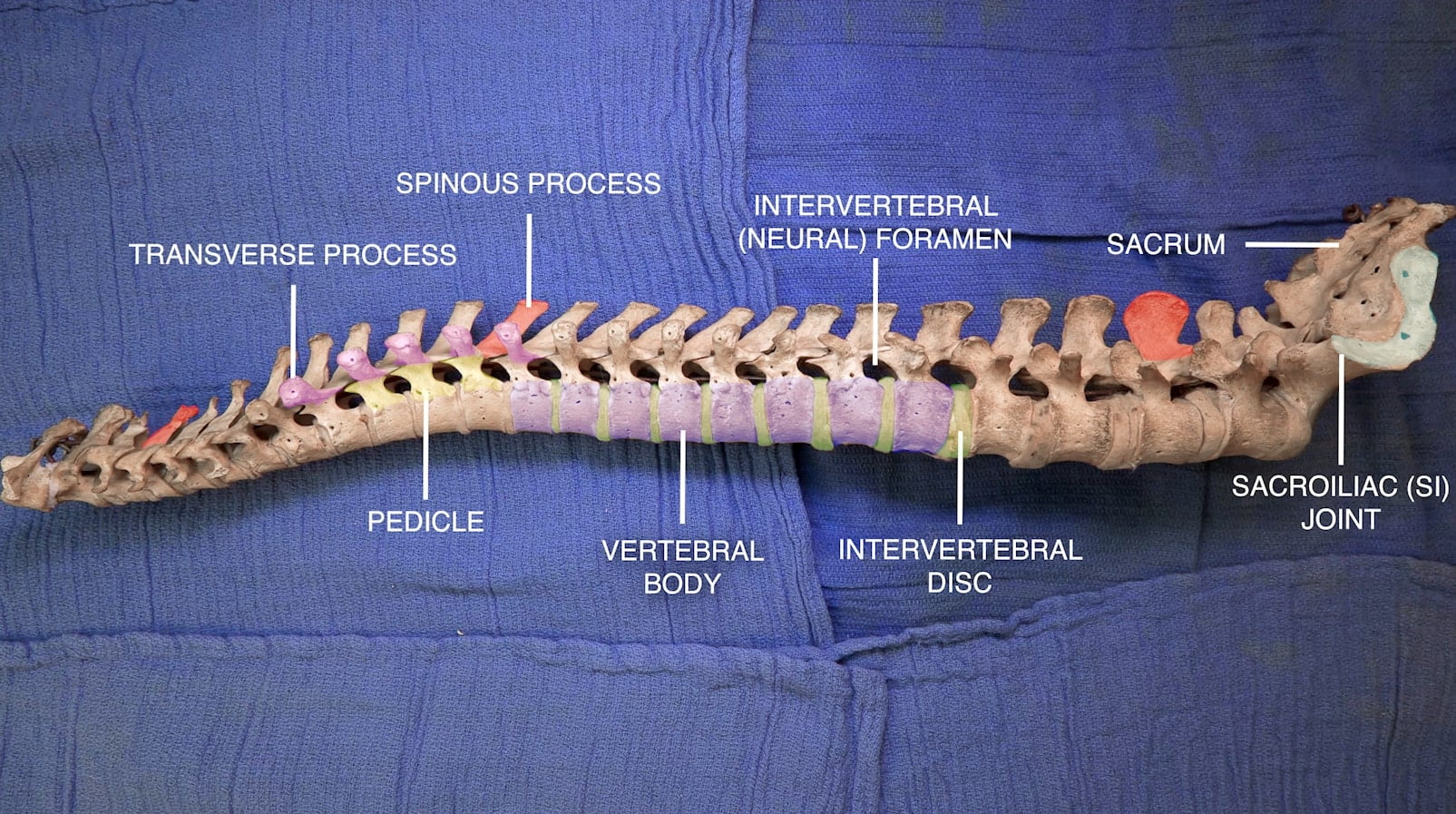
Vertebral Column
Spinal Column Part II
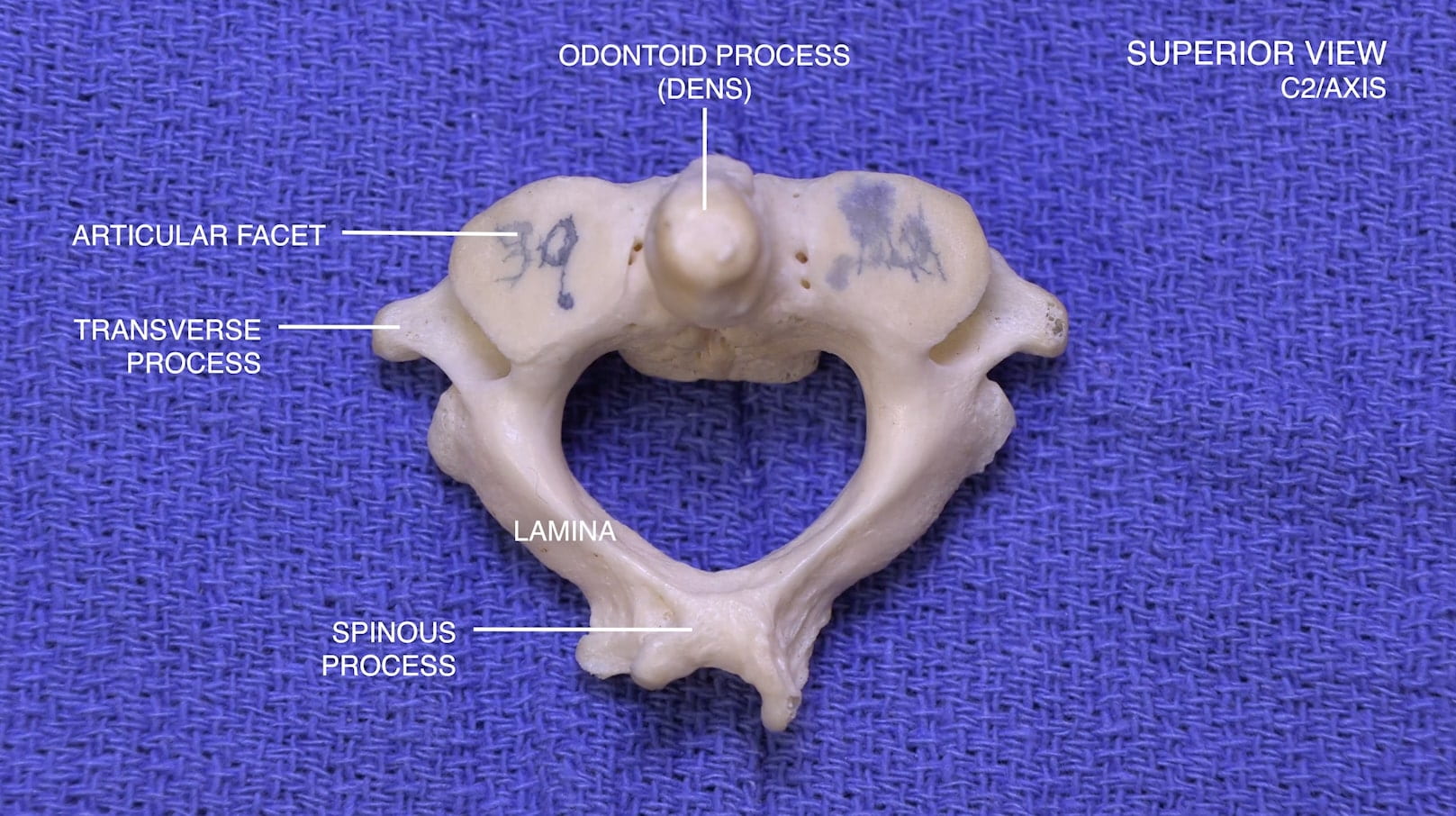
Vertebrae
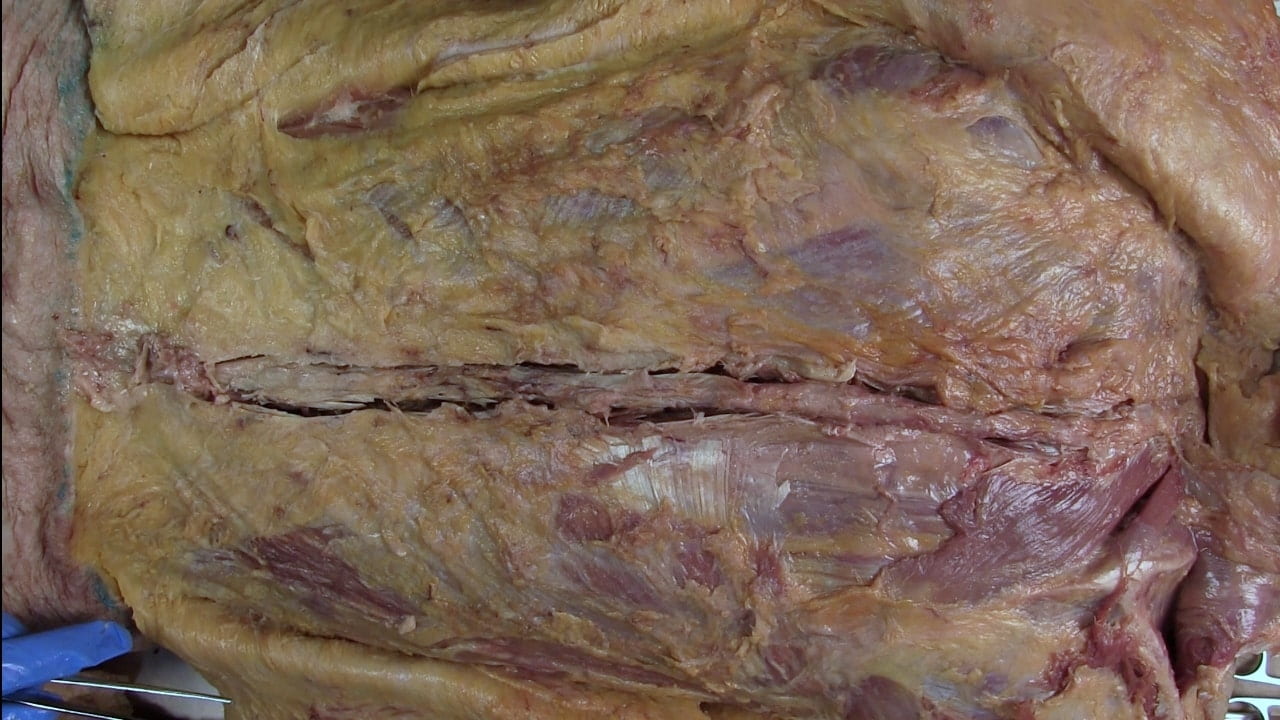
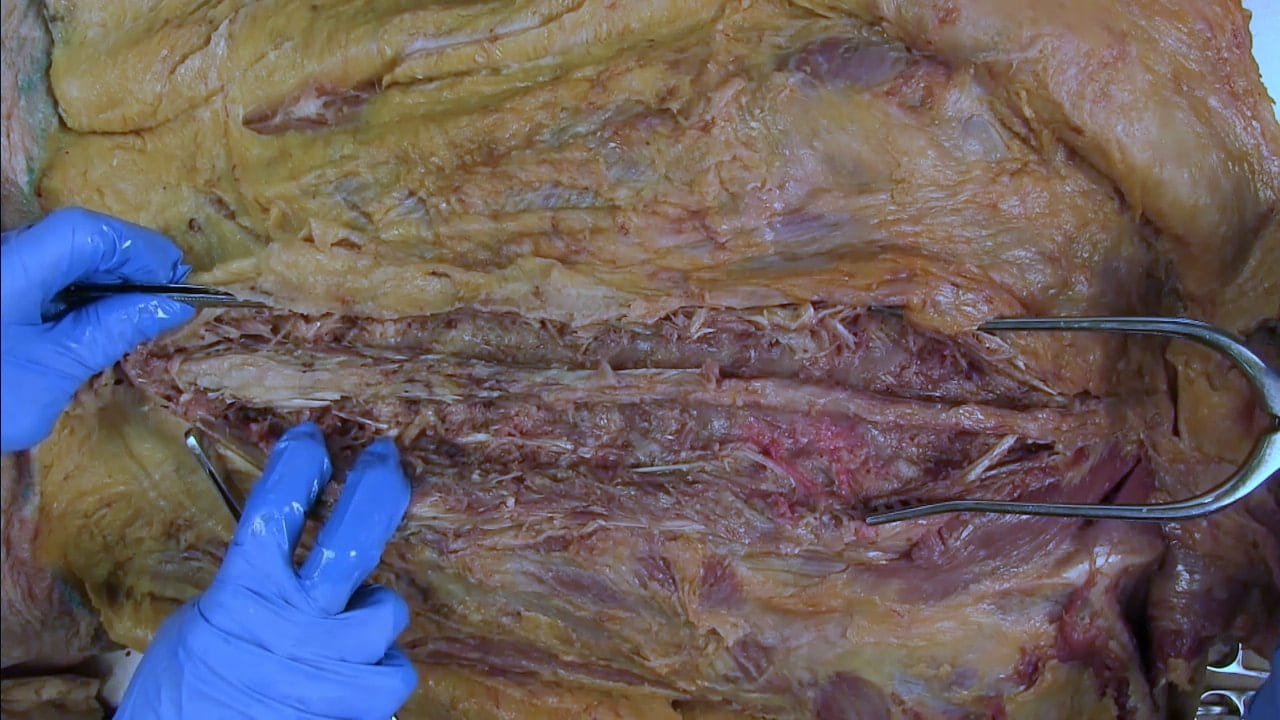
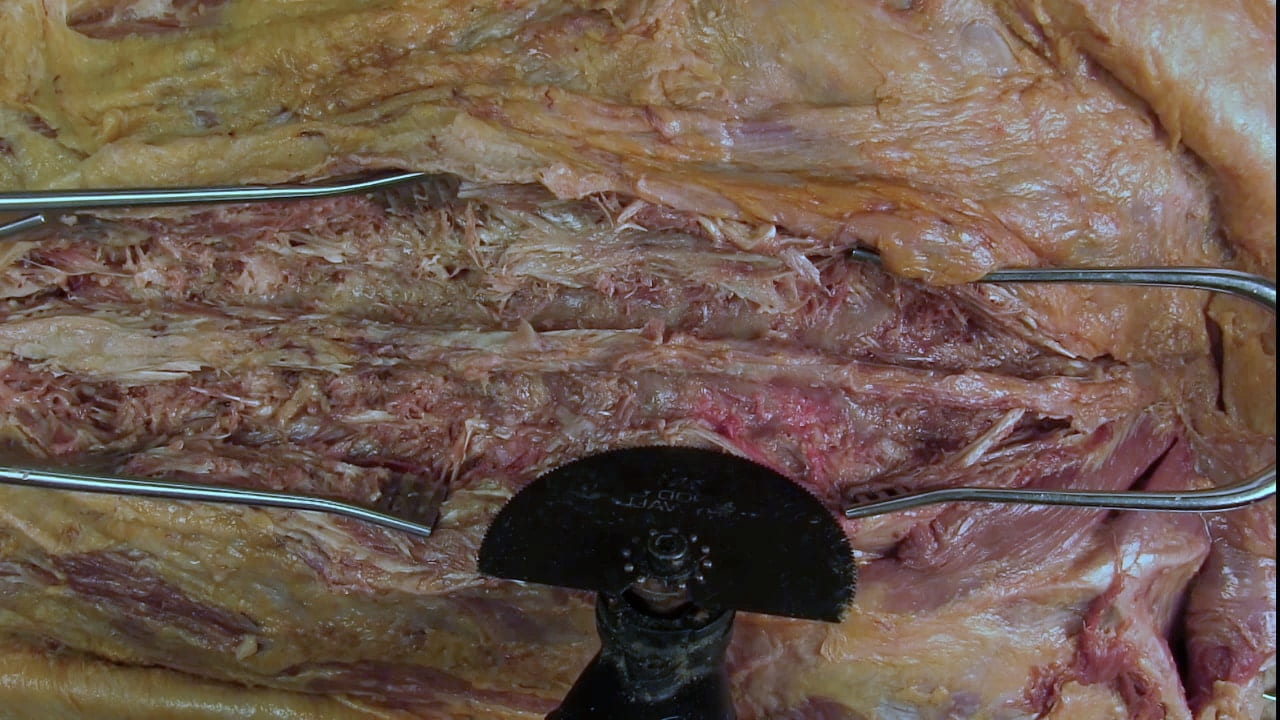
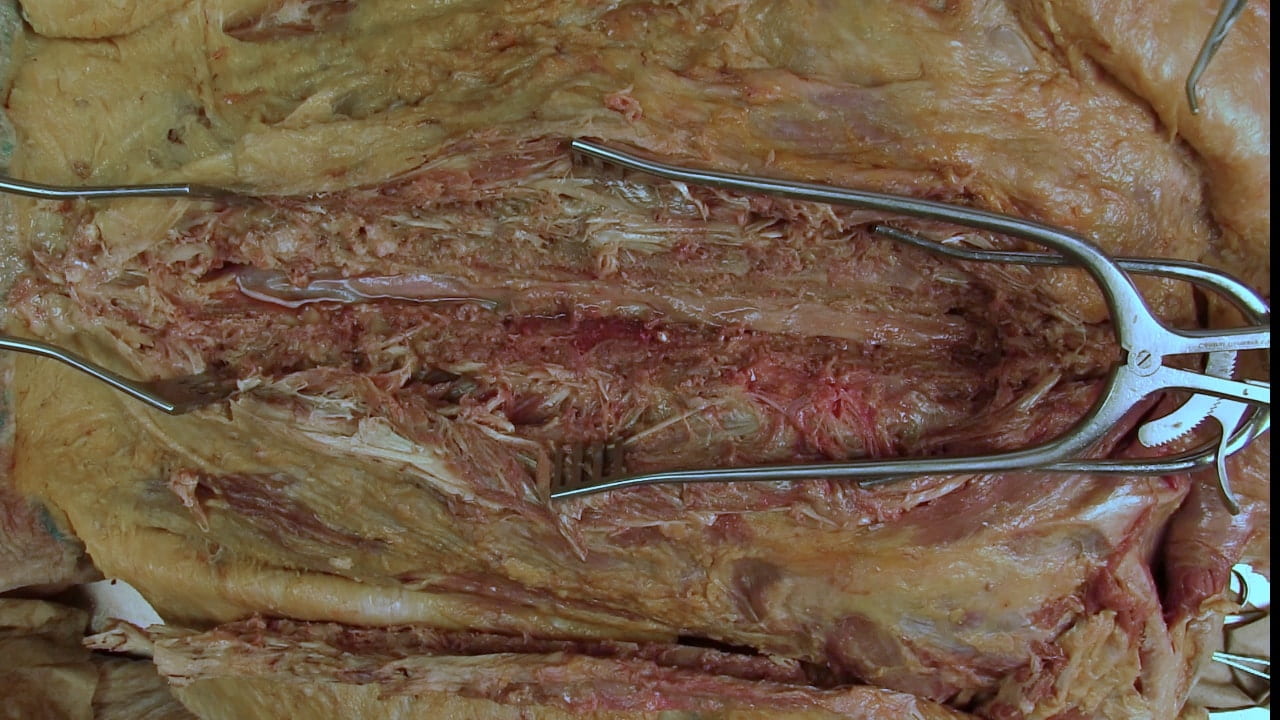
Expose Spine
Opening the Spine
Dorsal Brain and Spinal Cord
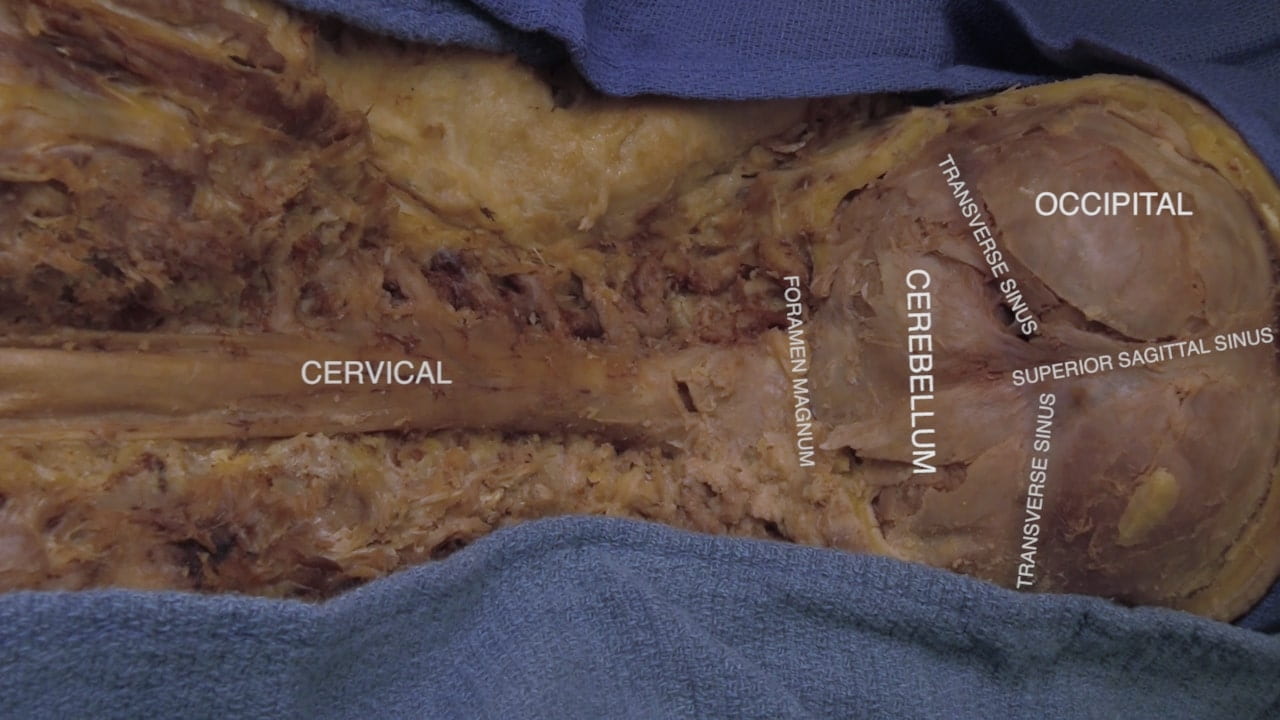
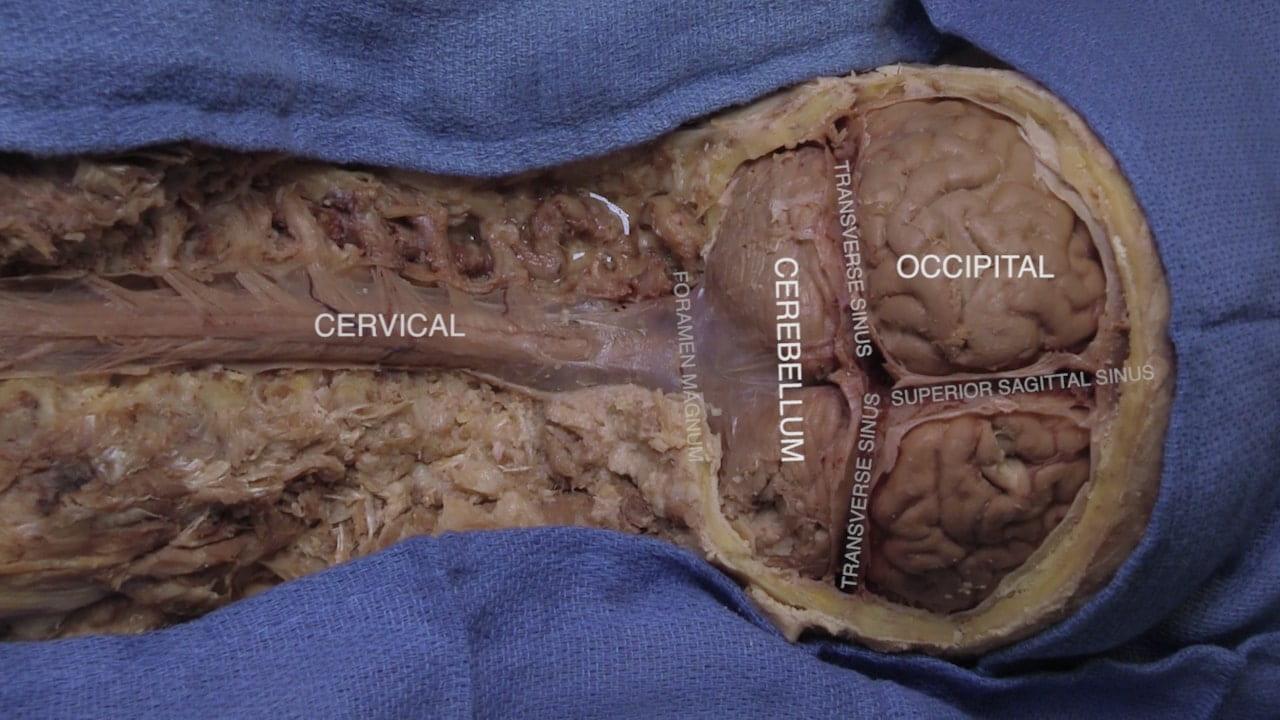
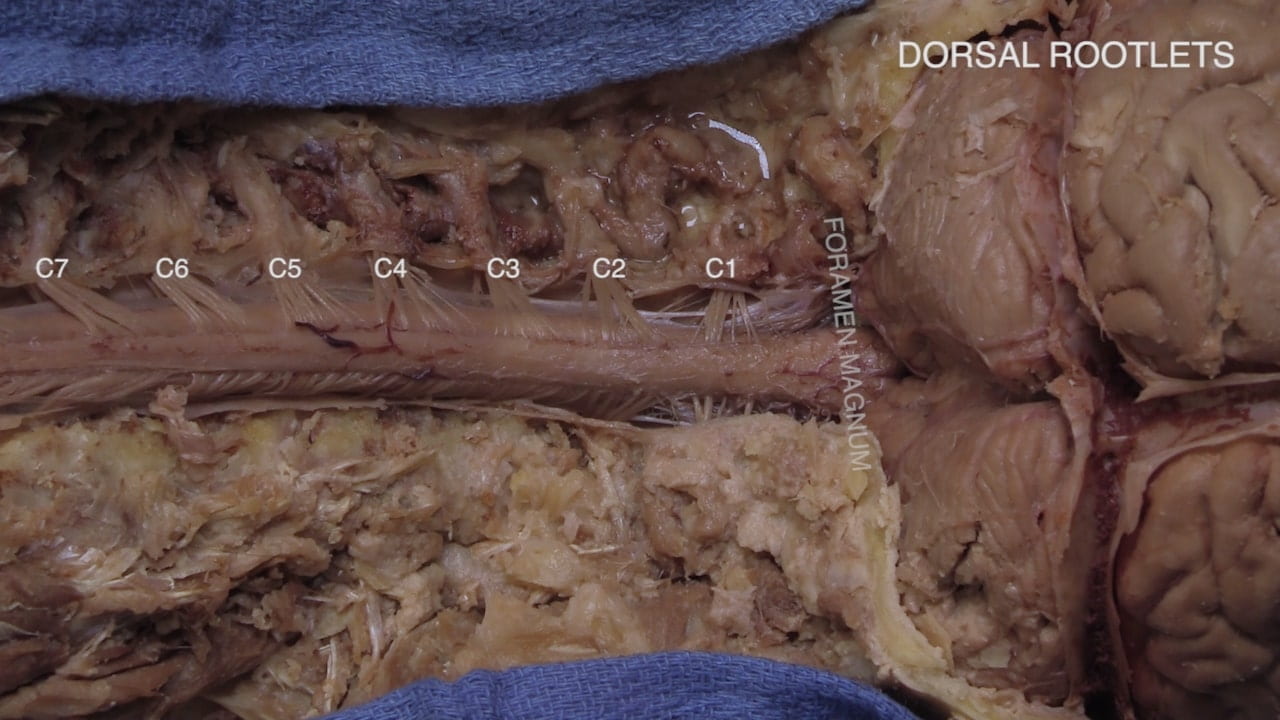
Exposing Cervical Spinal Cord and Posterior Brain
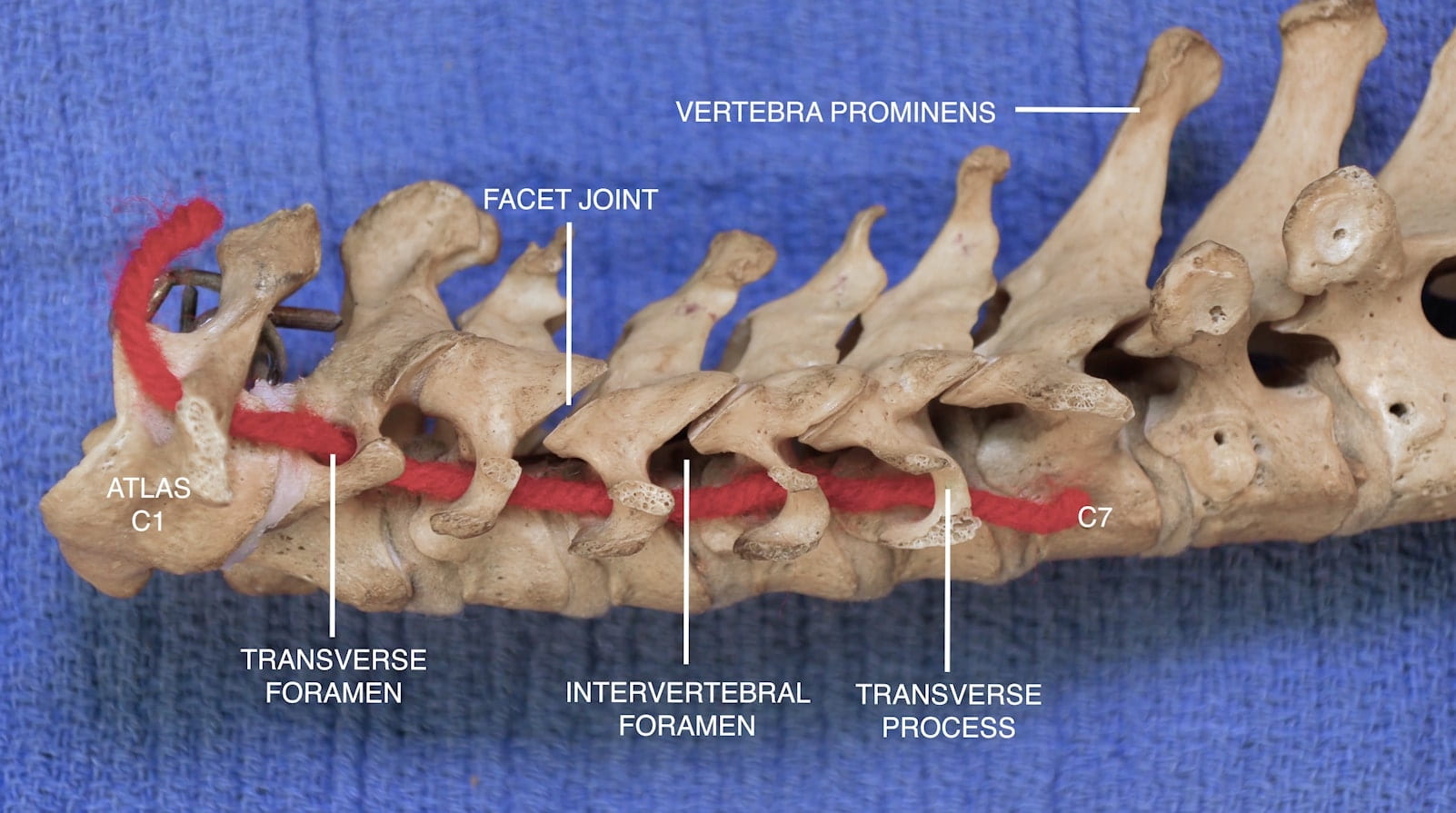
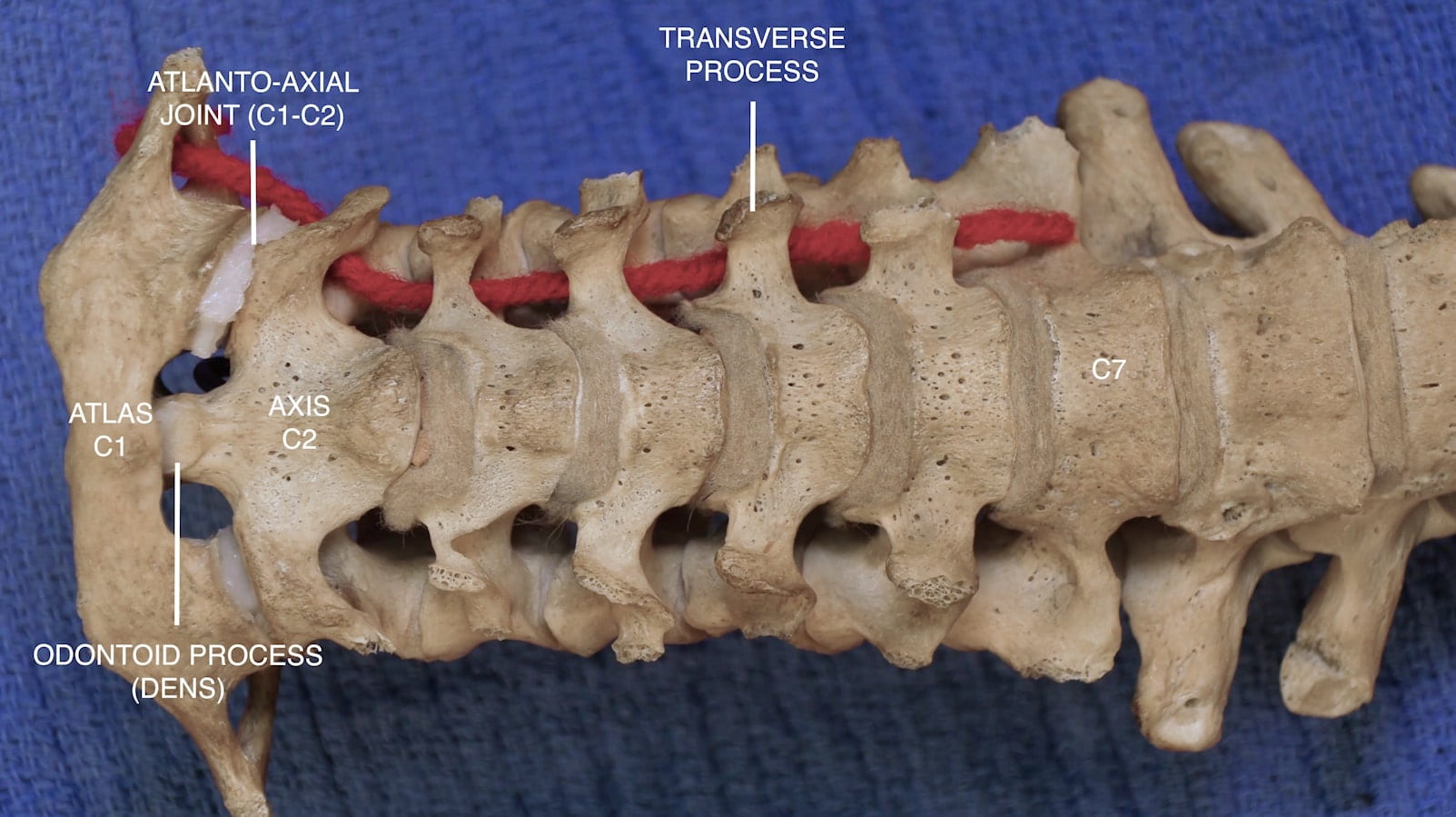
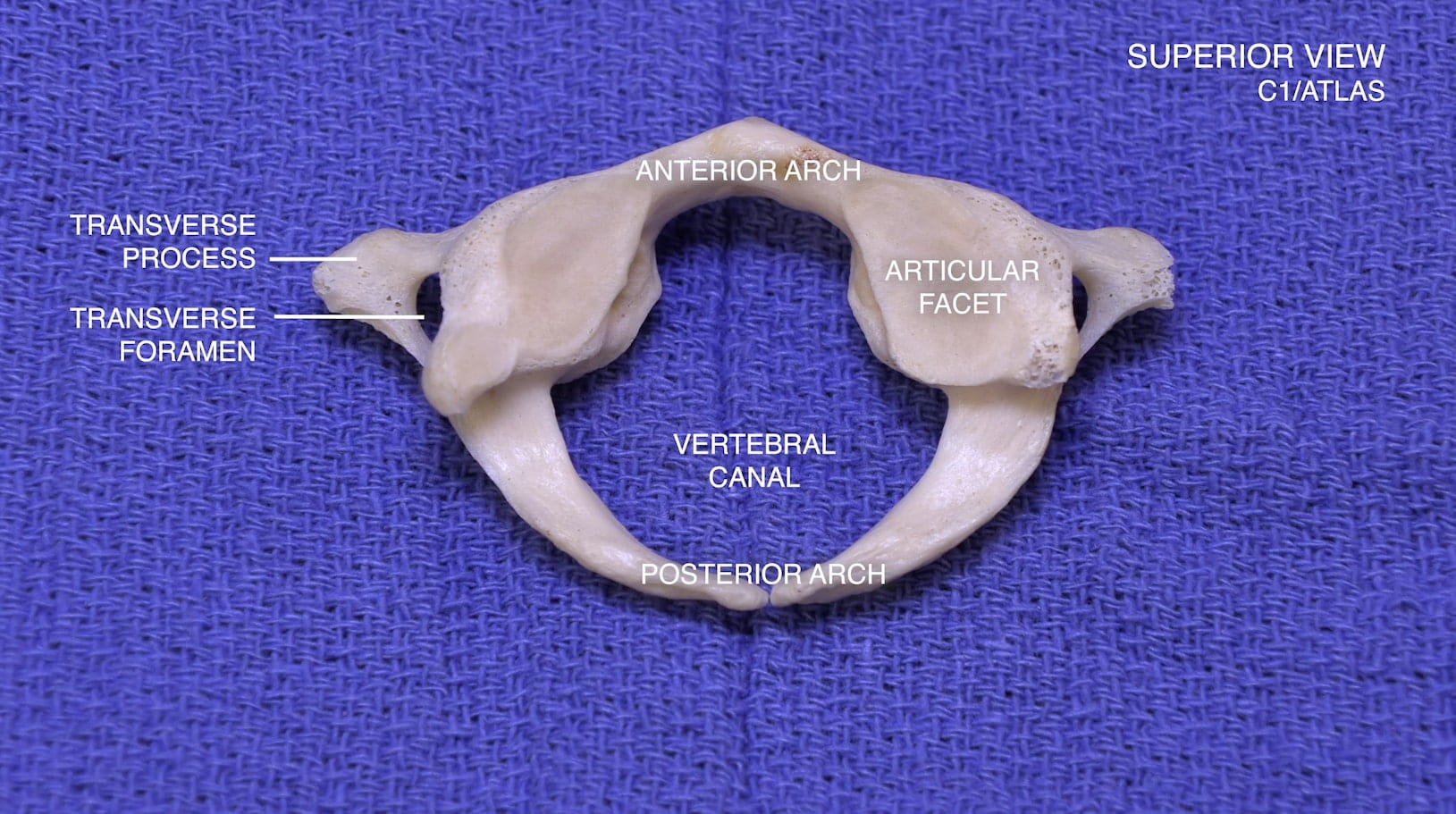
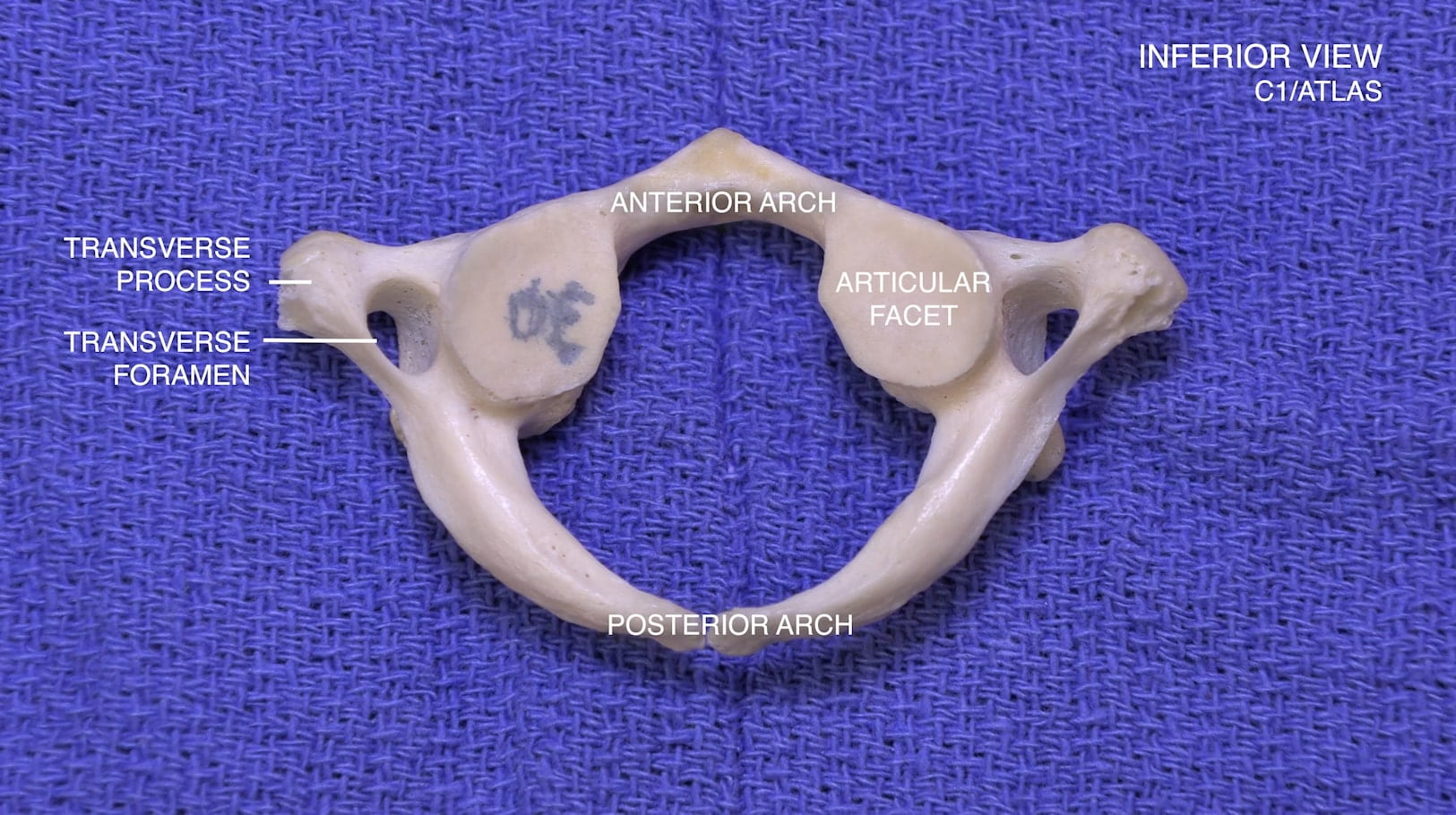
Craniovertebral Junction
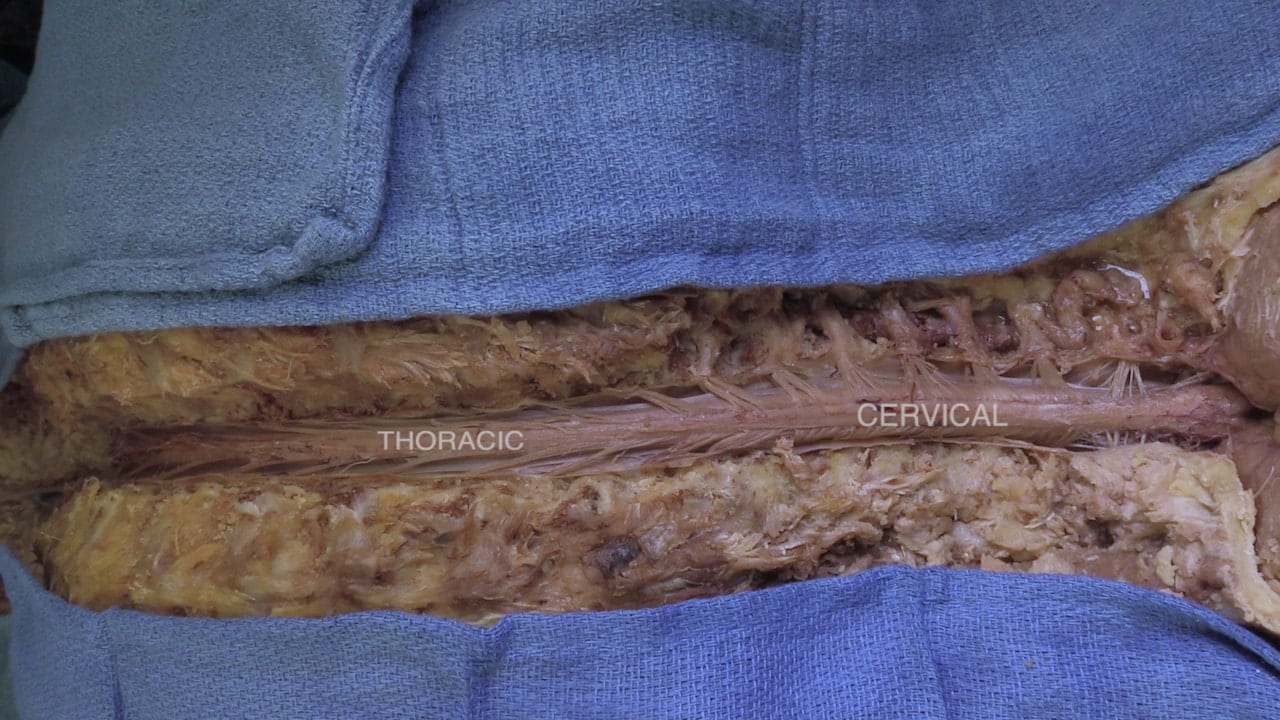
Spinal Cord Regions
Lumbar Puncture

Expose Ventral Spinal Cord
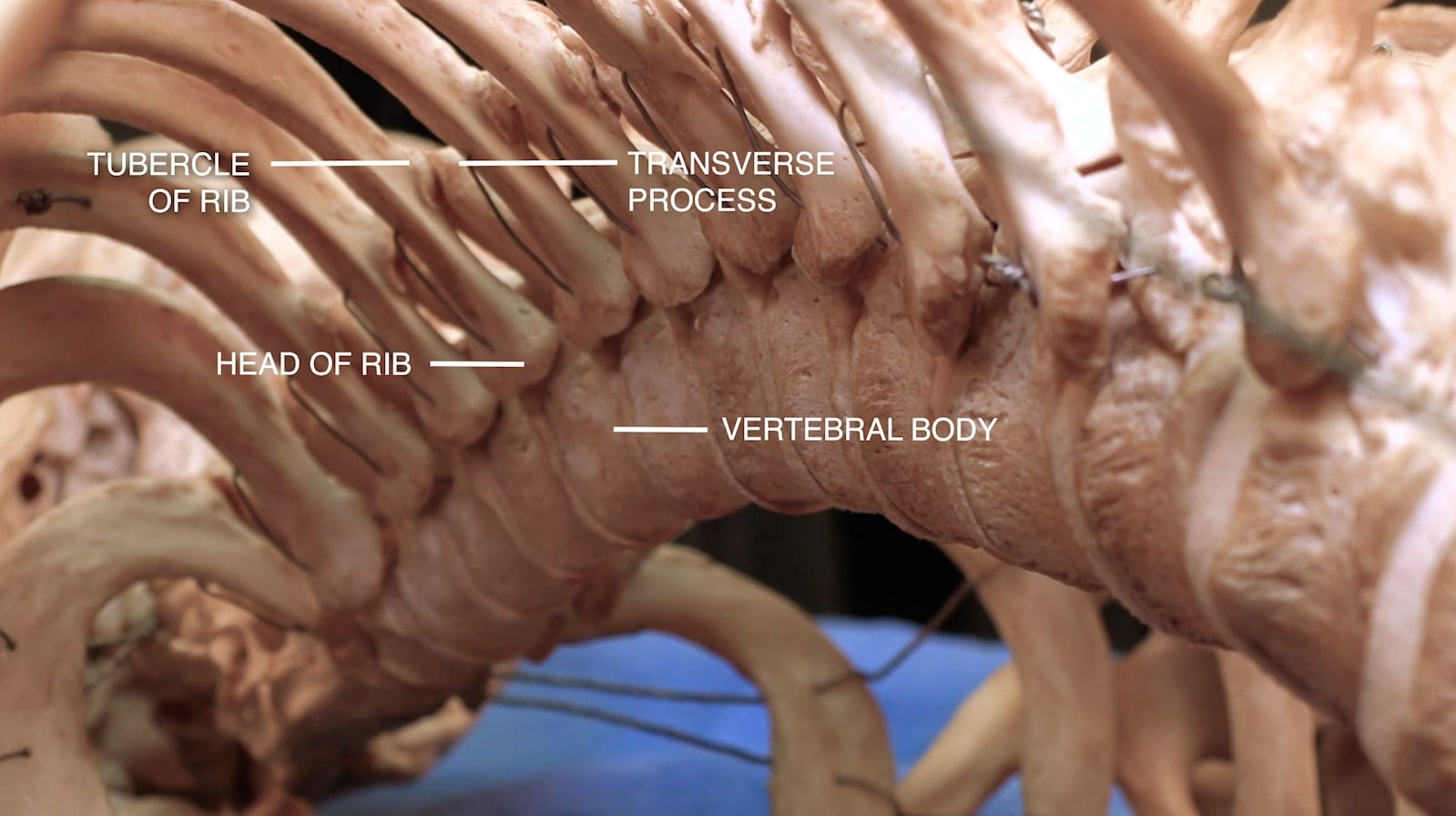
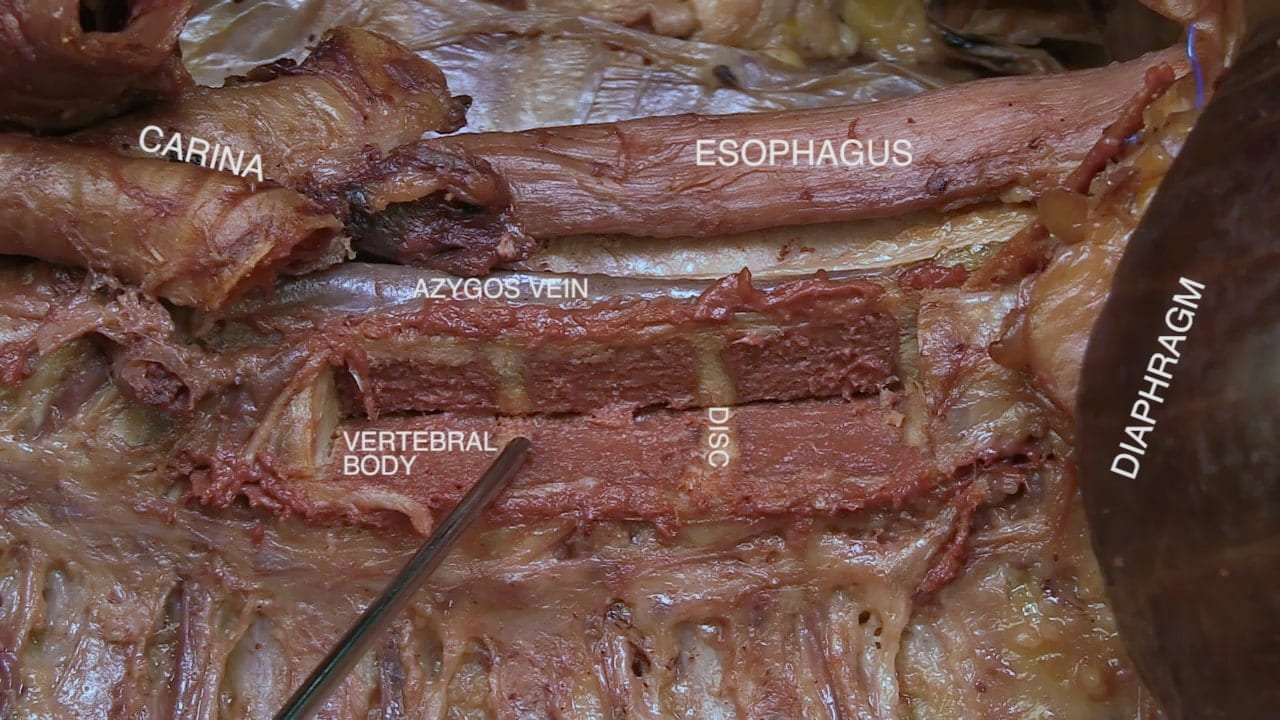
Vertebral Body In Situ
Anterior Thoracic Spinal Cord
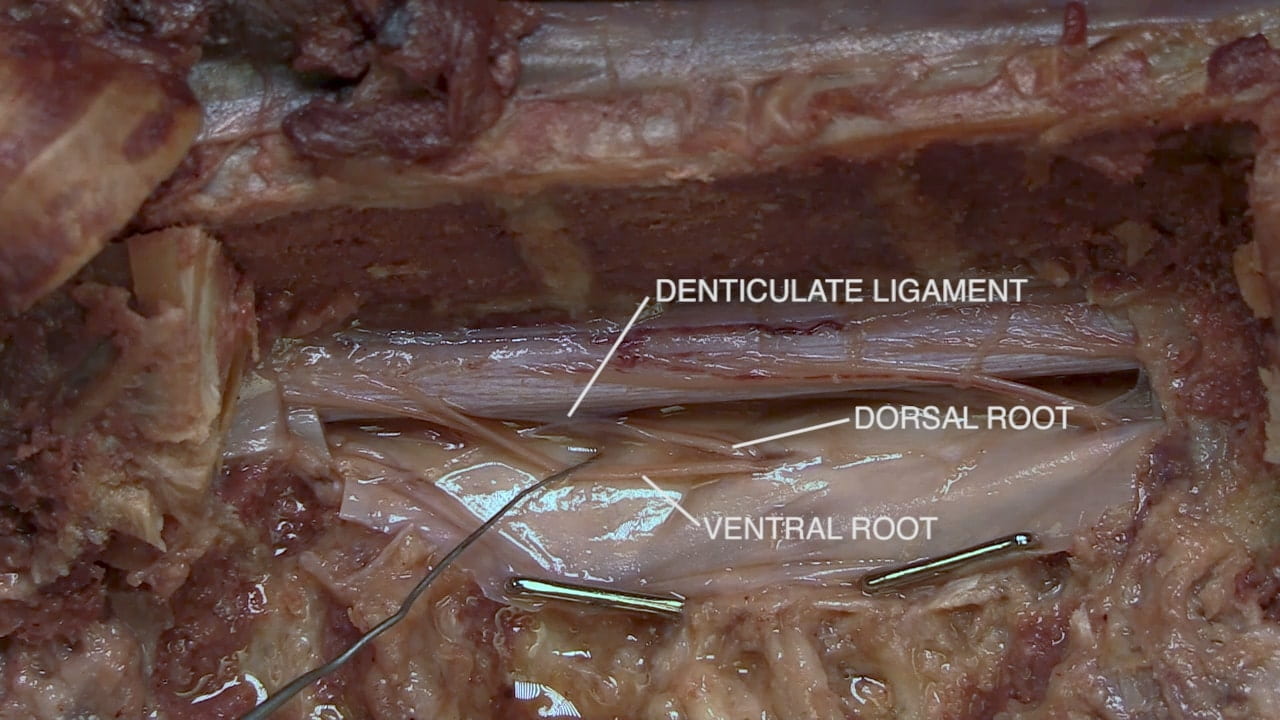
Ventral Spinal Cord
Anterior Spinal Cord
Removed Spinal Cord
Isolated Spinal Cord
3D – Atlas (C1)
3D – Axis (C2)
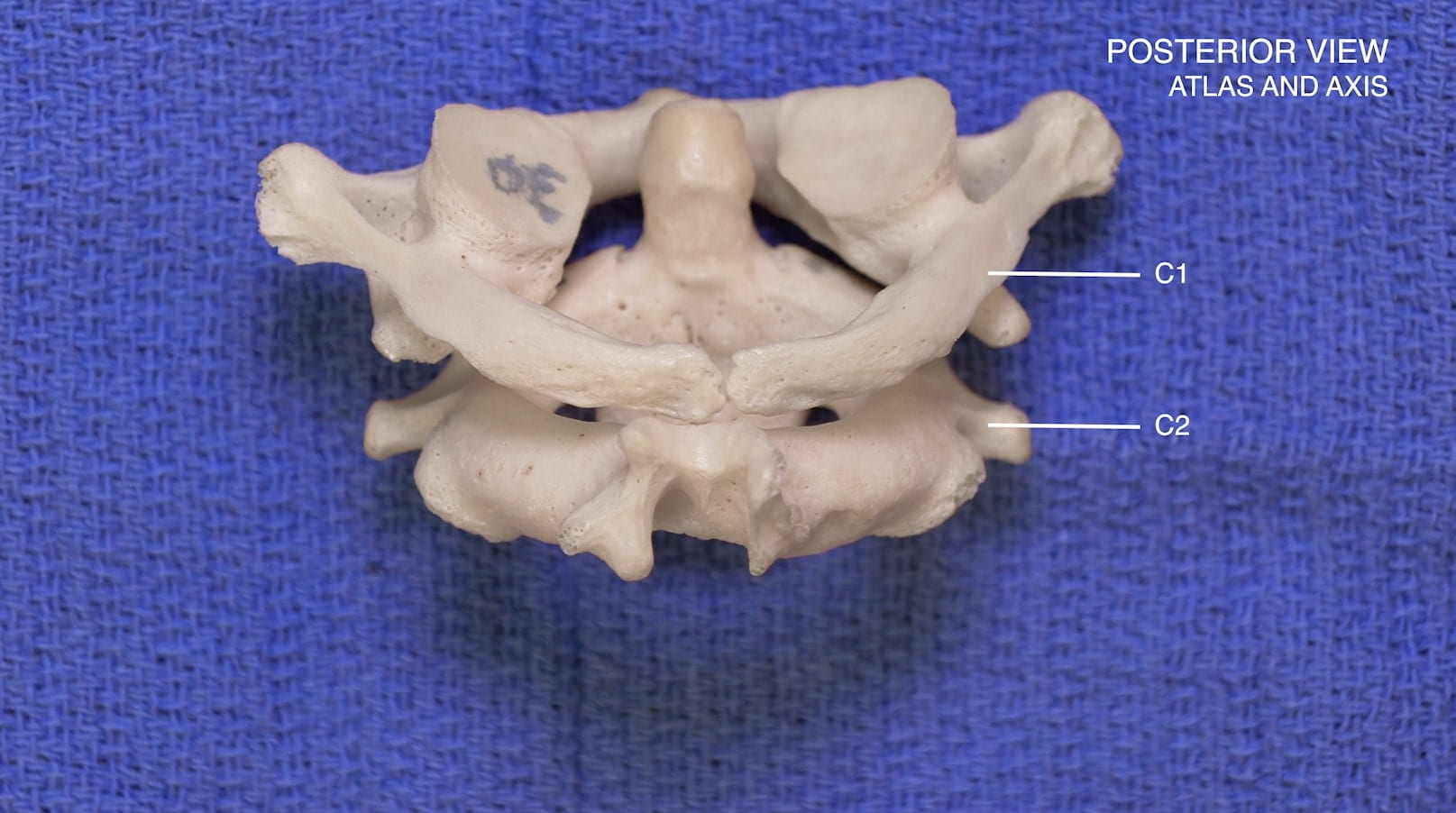
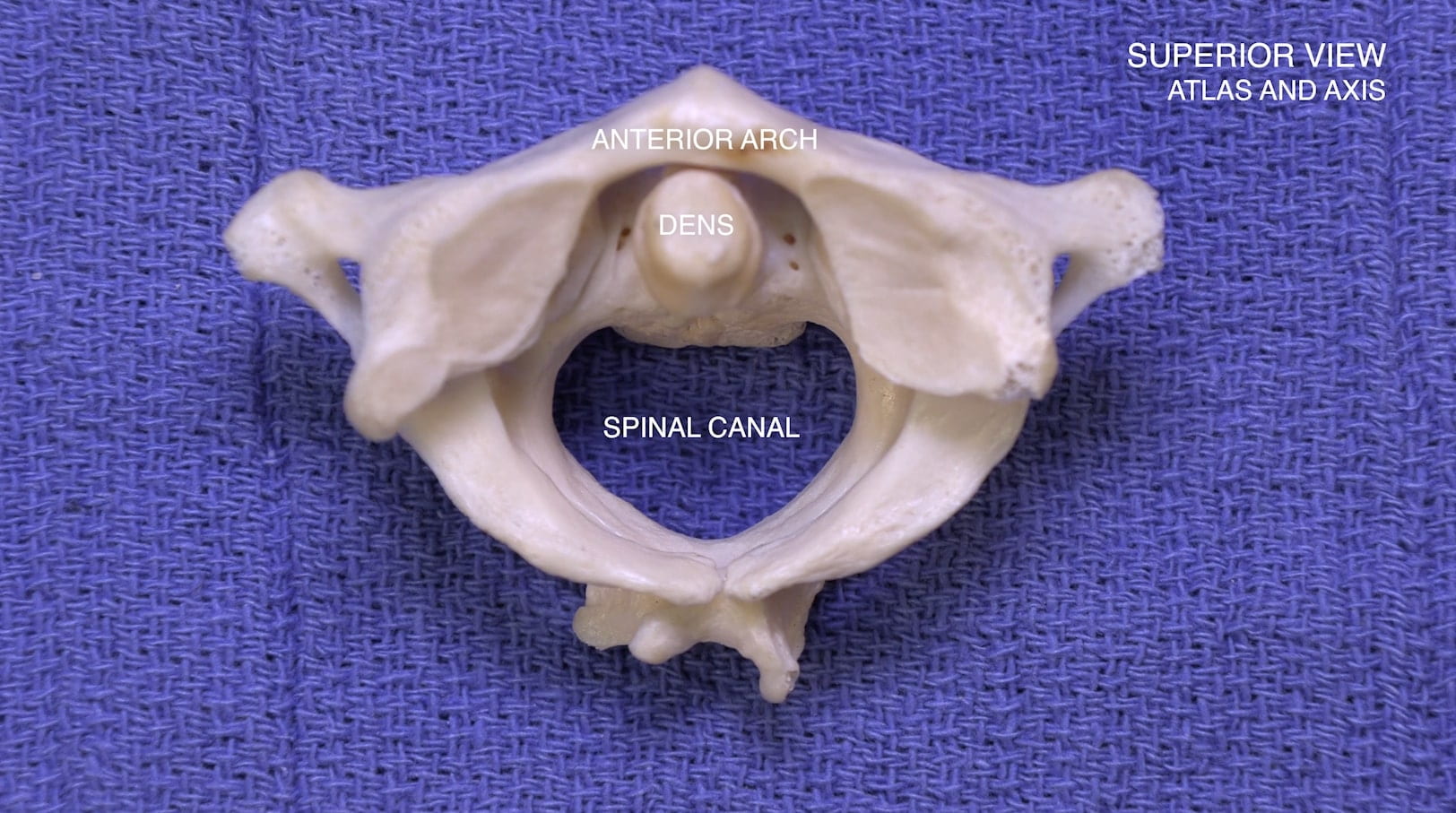
3D – Atlas and Axis
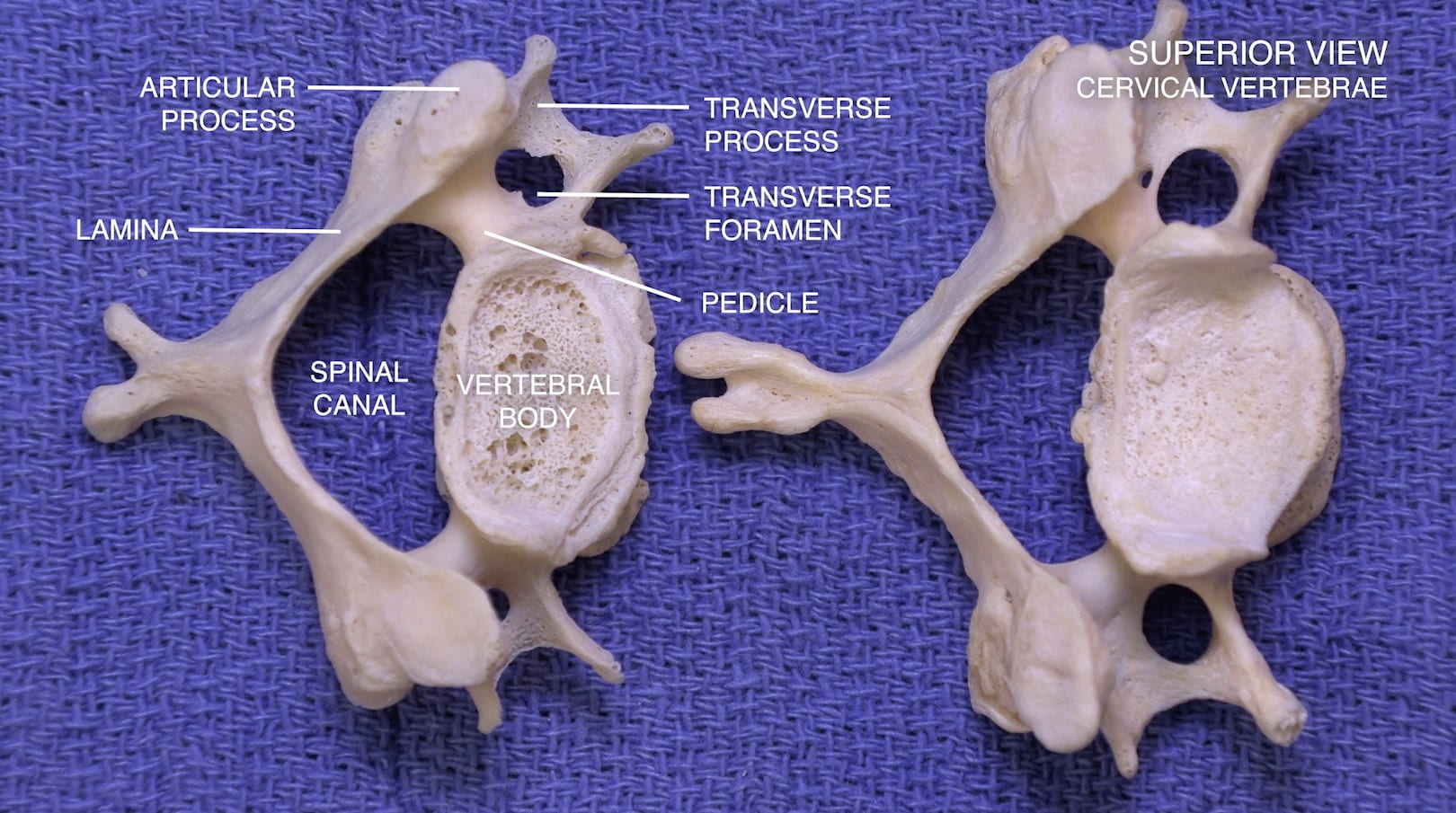
3D – Cervical
3D – Thoracic
3D – Thoracic Ligaments Model
3D – Lumbar
3D – Sacrum
Spine Clinical Correlations
Spine Clinical Correlations
Trauma/EM: Cervical spine injury (CSI): Traumatic injury to the spine is most commonly seen in young male adults; the cervical spine is the most affected region of the spine. The mechanism of injury is generally blunt in nature (e.g., during motor vehicle accident). Any patient with high-energy trauma should be suspected of CSI and placed in a cervical immobilizer collar to prevent further injury. Presentation of CSI varies depending on the patient and the nature of injury but may include midline neck pain, tenderness with palpation, stiffness, and decreased range of motion. Signs of neurologic involvement includes weakness or paresthesia (i.e., numbness, tingling, pins/needles) of the extremities. Patients with suspected CSI should undergo rigorous physical exam and neurological assessment inclusive of reflex, range of motion, sensation, and motor testing. After a thorough neurological evaluation, patients without symptoms of CSI or neurological deficits can have their cervical immobilizer removed (so-called C-spine clearance). Patients with concerning exam findings should receive x-ray. There are several classification systems for CSI; important criteria include level of injury, presence of fracture, and degree/localization of spinal cord injury.
Procedure: Spinal tap: Cerebrospinal fluid (CSF) is located within cerebral ventricular system and the subarachnoid space. Functionally, the CSF mechanically cushions the brain and transports nutrients and waste. Clinically, the CSF can be sampled through a lumbar puncture and analyzed in a laboratory for signs of infection, inflammation, hemorrhage, and malignancy. This is most done in suspected cases of meningitis. During an LP, patients are placed into a lateral decubitus position to maximize flexion of the lumbar spine and therefore expansion of the intervertebral spaces. The ideal point of insertion of the lumbar puncture needle is L3-L4 or L4-L5 interspace (Why? Think about state of spinal cord at this point). A commonly utilized landmark to find the L4-L5 intervertebral space is the imaginary line formed by the posterior superior iliac crest (Tuffier’s Line). As the needle is inserted, it will pass through several layers: skin, subcutaneous tissue, supraspinous ligament, interspinous ligament, ligamentum flavum (feel a “pop”), epidural space, dura mater (maybe another “pop”), arachnoid mater, and into the subarachnoid space. Once the subarachnoid space is reached, CSF will begin flowing. CSF pressure can be measured using a manometer (normal pressure: 6-25 cm H2O) before CSF collection (1-2 mL in 4 collection tubes) is performed.
Embryology: Spina bifida: The neural plate is the embryological precursor to the nervous system. This plate begins folding on itself to form the neural tube (by the 4th week of gestation) which will become the brain and spinal cord. This process (neurulation) is also critical for migration of somites, which will form the vertebral column. If somites do not properly form or migrate, a defect in the spinal column will occur (spina bifida). Spina bifida most commonly affects the lumbrosacral region. There are two forms of spina bifida: 1) spina bifida occulta which has minimal neural involvement and 2) spina bifida aperta which has varying degrees of neurological involvement and dysfunction. Neural tube defects are multifactorial, but folate-deficiency is a major environmental risk factor. Prenatal screening generally evaluates for high alpha-fetoprotein levels which are indicative of neural tube defects; subsequent ultrasound or amniocentesis can be performed to confirm the diagnosis. Spina bifida aperta generally requires surgical repair (unlike occulta).
Surgery: Discectomy: The spinal column consists of vertebral bones separated by intervertebral discs. These discs have two major components: a tough, outer ring (annulus fibrosus) surrounding a gel-like inside (nucleus pulposus). Degeneration or trauma may facilitate protrusion of the nucleus pulposus through a weakened annulus fibrosus. This disc herniation can press on nerves causing paresthesia, pain, and weakness. To address this, a discectomy can be performed to relieve pressure on affected nerves. Traditionally, this entails a laminotomy (cutting lamina of vertebral bone; you will do this in lab!) to improve visualization of the region followed by gentle retraction of intervening spinal nerves and removal of the herniated disc segment. Advances in imaging and surgical instrumentation now enable endoscopic- and micro- discectomies. Disectomy is indicated in patients with cauda equina syndrome, persistent pain in spite of 6-8 weeks of conservative therapy (rest, medication, and therapy), or new neurological deficits.
Anatomical Variation: Vertebral Arteries: The vertebral arteries (VAs) are classically described as 1) arising from the subclavian arteries bilaterally, 2) traveling superiorly and entering the transverse foramina of the 6th cervical vertebrae, and 3) merging to form the basilar artery. However, variations in the VA are common. Occasionally, the VAs may arise from the aortic arch (most common variation). The left and right VAs may also be asymmetric in size; the larger one is dominant. VAs may also enter the transverse foramina at C3, C4, or C5.